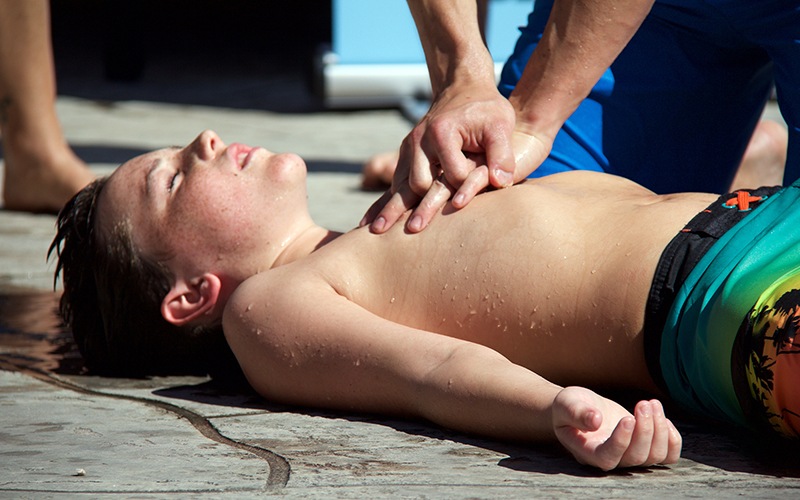
What is "social" resuscitation and the link with paediatric CPR
When you resuscitate a patient, you are not resuscitating the patient only. You are resuscitating people connected to him/her: family, for example. This is what has been called “social” resuscitation.
As Dr Ruth Parsell, working on the CareFlight Rapid Response Helicopter in Sydney, states on Care Flight Collective, that “social resuscitation” is a term generally used in dire situations. In particular with paediatric patients.
These are parts of the resuscitation that have no algorithm, no protocols. How can those parts be improved? As Dr Parsell says, there are experiences we do not want to gain. Ever. One case is a paediatric resuscitation, as announced at the beginning.
We all wish we didn’t see these cases but if they continue to occur then we will continue to do our best to serve the needs of both the patients and their families. […]
The best way to do both would be to have the “miracle” recovery. The “against all odds”, the “everything was against them”… the full recovery of a child who has had a terrible insult. The drowning, the fall, the pedestrian, the horse riding accident… all the terrible insults we see and all those mechanisms of injury that can potentially cause an early cardiac arrest or a moribund child.
Instantly we think of our algorithms, our protocols, our list of reversible causes and the sequence of steps we might take when we arrive at the scene. We hear the age, we think about weights, sizes, drug calculations. None of this should ever change and I’m not suggesting it should.
Don’t know why, but treating a kid is always a desperate and frustrating state of mind. It is not easy to explain the family the heart of your kid stopped beating and you are trying to re-start it.
What if it was just a kiss before the transport? What if the family could have a little more from us? What if we suggested getting their daughter’s favourite teddy or blanket from the house? Just to fill their arms for the trip to hospital, to stop Mum’s hands from relentlessly wringing or something to give her tears a soft landing when they fall. […]
Now I think that the social resuscitation needs to start earlier. A more conscious and deliberate effort. Maybe not every time. Not when you can feel yourself buckling under the cognitive load. Not when your emotions are so close to the surface you can’t get the words out. Not when the scene is like a powder keg and you might just be putting people at risk.
But in those paediatrics cases we need to make a conscious effort to find a window, even where the algorithm is crowding us a little more. That might be the part of the resuscitation that isn’t futile for those left behind.
Try the explanation. Try the kiss. Wait for that teddy. Just try it and let’s see if it improves our social resuscitations. It might even just improve things for all of us.



