What is ocular myasthenia gravis and how is it treated?
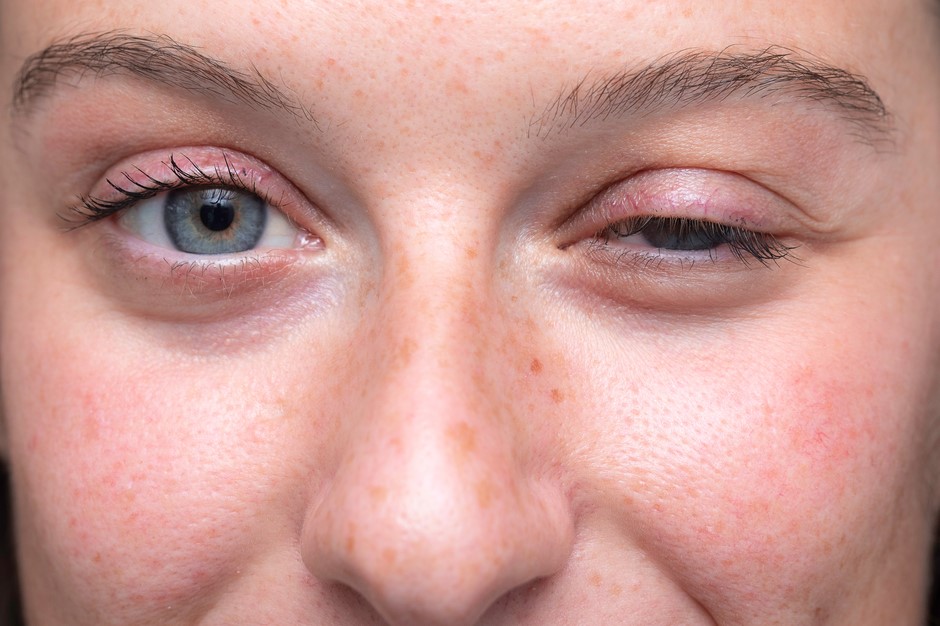
Ocular myasthenia gravis is an autoimmune disease involving eyes and eyelids
Ocular myasthenia gravis is a form of myasthenia gravis limited to the muscles of the eyes and eyelids
Myasthenia gravis is an autoimmune disease resulting from a malfunction of the immune system.
It occurs when our body produces auto-antibodies that interfere with the transmission of muscle contraction.
This mechanism disrupts the communication between nerves and muscles causing episodes of extreme weakness.
Affected persons have drooping eyelids or double vision.
Ocular myasthenia is a subtle disease, often not identified at its onset, as symptoms may be initially mild and easily attributable to other causes.
Ocular myasthenia gravis, people at risk
This disease affects women and men equally and can appear from adulthood onwards.
People who already suffer from other autoimmune diseases such as rheumatoid arthritis, systemic lupus erythematosus (SLE), scleroderma and thyroiditis are more likely to develop it.
Symptoms of ocular myasthenia gravis
In around 40% of people with myasthenia gravis, the onset symptoms affect the eye muscles, with up to 85% of patients experiencing this problem over the years.
In 15% of cases, only the eye muscles are affected, without systemic involvement.
The typical symptoms of ocular myasthenia are 2:
- double vision (diplopia)
- drooping eyelid (ptosis).
Double vision
The presence of diplopia or double vision depends on the involvement of a single extraocular muscle which, not working in conjunction with the other eye, causes this annoying sensation of double vision.
Drooping eyelid characteristic of ocular myasthenia gravis
Palpebral ptosis or drooping eyelid, on the other hand, results from impairment of the normal functioning of the elevator muscle of the upper eyelid.
Eyelid drooping can affect one or both eyes, to varying degrees throughout the day.
Diagnosis
Diagnosing ocular myasthenia is not always easy.
For this reason, doctors have to resort to various diagnostic tests.
A medical examination and simple tests are essential.
The test
In the presence of diplopia and ptosis, the patient is asked to exercise the eye muscles until they become tired.
Then the doctor may apply an ice pack to the eyes, or ask the patient to lie down in a dark room for a few minutes with his eyes closed. If the ptosis reduces after the examination, doctors suspect ocular myasthenia.
Examinations
Confirmation of the pathology comes through
- blood tests that aim to detect antibodies specific to the disease;
- electromyography, which involves inserting a needle into a muscle to record its electrical activity;
- computed tomography (CT) or magnetic resonance imaging (MRI) of the chest to assess the thymus, a gland in the chest, to determine if a thymoma (thymus tumour) is present.
Assessing the thymus is important because about 65% of those with myasthenia gravis have an enlarged thymus and 10% have a thymic tumour. Unfortunately, about half of these thymomas are cancerous (malignant) and must be removed.
How to treat ocular myasthenia gravis
At present there is no specific cure, only a series of symptomatic treatments involving the administration of:
- cholinesterase inhibitors, such as pyridostigmine, which improve symptoms;.
- corticosteroids and immunosuppressants (such as azathioprine, methotrexate and cyclosporine), which modulate the immune response and make self-antibodies, responsible for blocking muscle contraction, less effective.
Surgical removal of the thymus can help control symptoms, although it is still controversial why it is only effective in some patients.
Patients are prescribed eye and vision aids such as:
- eye patching for double vision;
- the use of crutch glasses for ptosis.
Both solutions can improve patients’ quality of life.
Read Also:
What Is Ocular Pressure And How Is It Measured?
Opening The Eyes Of The World, CUAMM’s “ForeSeeing Inclusion” Project To Combat Blindness In Uganda


