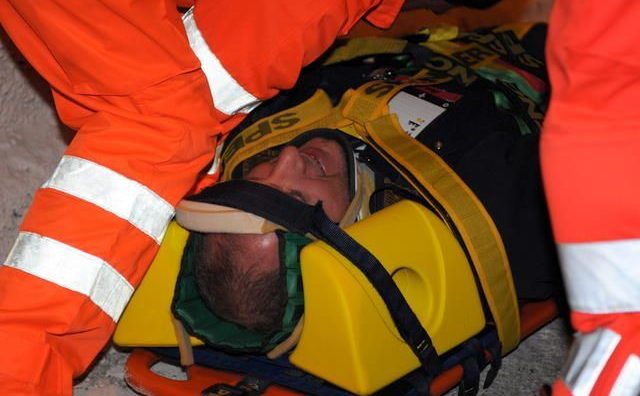
What to know about the neck trauma in emergency? Basics, signs and treatments
Neck trauma is the most complex injury to treat for different reasons. In particular, in the neck are based most vital parts. In addition, patients with neck trauma may appear stable and only afterwards the injury causes problems and complications.
This is why is essential to know absolutely well the neck, how it is made, what are the signs that must make us suspect a neck trauma, which are the zones to treat according to the disease of the patient, and so on. So, what are the important aspects a prehospital operator must bear in mind to discover or/and treat a neck injury?
_______________________________________________________
Author: Amaan Siddiqi, MD (Senior EM Resident, Brooklyn Hospital Center)
Edited by: Alex Koyfman, MD (@EMHighAK) and Justin Bright, MD
Basics of Neck Trauma
The neck is a particularly tricky area of assessment and management in the trauma patient, as it is the location for many vital structures. Concern for vascular, neurologic, digestive tract and airway injury are of paramount importance in the evaluation of these patients, as all can be life-threatening. Oftentimes, the neck trauma patient may appear stable, only to have delayed injury found later, causing increased morbidity and mortality. Neck trauma can be split into penetrating injury and blunt injury.
The neck is divided into 3 zones, which become important in evaluating and managing these patients, especially with regard to the structures lying within each division.
Zone I (base of the neck) – below the cricoid cartilage (to the sternal notch): mediastinal structures, thoracic duct, proximal carotid artery, vertebral/subclavian artery, trachea, lung, esophagus
Zone II (mid-neck) – from the cricoid cartilage to the angle of the mandible: carotid/vertebral artery, larynx, trachea, esophagus, jugular vein, vagus and recurrent laryngeal nerves
Zone III (upper neck) – above the angle of the mandible: distal carotid artery, vertebral artery, distal jugular vein, salivary/parotid glands, CNs 9-12.
The struggle with neck trauma lies in the different zones of the neck. Zones I and III are difficult to access and to manage in the operating room, with Zone I injuries at the highest risk. Zone II is the most exposed zone, and is consequently the most likely to be injured. However, Zone II injuries also have the best prognosis because there are larger areas of exposure, allowing for easier proximal and distal control.
The incidence of penetrating trauma is 0.55-5% of all traumatic injuries. The major mechanisms are GSW, stab wounds, and shrapnel. Stab wounds and lower-velocity GSW cause a 50% lower incidence of clinically significant lesions.
Blunt neck trauma is even more uncommon than penetrating neck trauma. The majority of blunt neck trauma is from MVCs, as well as assault and strangulation. The major issue with blunt trauma of the neck is in missed or delayed diagnosis.
Stable patients should be evaluated for “hard” and “soft” signs. “Hard” signs indicate the need for emergent management, i.e. surgical consult and operative intervention. “Soft” signs indicate close observation and reevaluation, though not necessarily surgical intervention.
Soft Signs
- Hemoptysis or hematemesis
- Oropharyngeal blood
- Dyspnea
- Dysphonia or dysphagia
- Subcutaneous air or mediastinal air
- Chest tube air leak
- Nonexpanding hematoma
- Focal neurologic deficits
Hard Signs
- Expanding hematoma
- Severe active bleeding
- Shock not responding to fluids
- Decreased or absent radial pulse
- Vascular bruit or thrill
- Cerebral ischemia
- Airway obstruction
Management
Start with your ABCs while following ATLS guidelines, as in any trauma situation, with surgical consult at the bedside. We will concentrate on the specific injuries seen in neck trauma that are often encountered, including those easily missed.
Airway + Breathing
Physical signs that warrant immediate airway management include stridor, respiratory distress, shock, or rapidly expanding hematoma. In near-hanging or strangulation victims, you should maintain a very low threshold for intubation. Furthermore, these patients have a propensity to develop pulmonary edema and ARDS.


