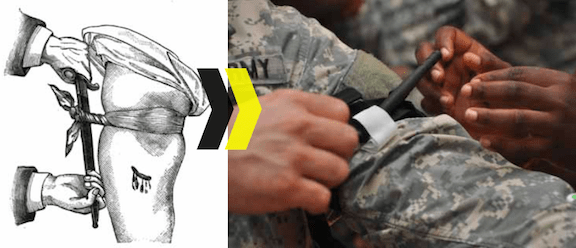
Tourniquets saves lifes? Maybe
FROM EMERGENCY PHYSICIANS – It is an atypical Saturday in your busy Level One trauma center as, fortunately, the knife and gun club seems to be taking the day off. You’ve just gotten a quick bite to eat when you hear the radio go off. EMS is bringing in a police officer shot in the thigh during a SWAT raid. The report is that he has an entrance wound in the upper mid-thigh with these vital signs: blood pressure 100/60, heart rate 120, respiratory rate 22, and 98% on room air. On the phone, the paramedics indicate that the bleeding is controlled with a tourniquet.
As the 40-year-old patient arrives in the ER, he is mildly diaphoretic, with a pulse of 100 and the same blood pressure reported in the field. As he’s wheeled into the trauma room, you do not see any obvious signs of active bleeding. You start your primary survey, and after establishing an intact airway and breathing, focus on the patient’s circulation.
But then the general surgeon covering trauma arrives and starts to yell at the paramedics about the dangers of putting a tourniquet on the patient, asserting that they may have put the patient in danger of losing his leg. Then the SWAT officer chimes in, stating he was the one who actually placed the tourniquet. He adds that he has just received training in the latest Tactical Combat Casualty Care guidelines, and now all SWAT officers are carrying tourniquets. The surgeon looks confused, and you realize you will need to have a talk with him after the shift.
The Past is Past
In the last several years, the United States military has gathered substantial evidence on the safety benefits of using tourniquets [1,2,3]. However, many physicians still may be hesitant to use this potentially lifesaving device. The chief concern: A tourniquet can induce ischemia in an already at risk extremity, which may lead to an unnecessary amputation [2]. This belief first developed in World War I when evacuation to surgical care took up to 18 hours and was re-enforced in World War II. Prolonged evacuation times and reliance on improvised tourniquets meant surgeons often saw survivors who may have not needed a tourniquet. Those that died in the field from simple extremity hemorrhage just never made it to the surgeon. In his 2012 article on the history of the tourniquet, John Kragh pointed out that, in several instances in war zone conflicts where the use of the tourniquet was criticized from these conflicts, there was a paucity of evidence to support those positions [2].
This bias, perpetuated in the surgical literature, is perhaps best put into perspective by New Zealand surgeon Douglas Jolly, who succinctly said that “more limbs and lives are lost at the front from the improper use of the tourniquet than are saved by its proper use [4].” Other observers have characterized the tourniquet as “an invention of the Evil One [5].”
READMORE ON EMERGENCY PHYSICIANS


