Wound care guideline (part 1) - Dressing overview
When faced with a complex instance of wound care, many first time or novice clinicians will ask, ‘What wound is this? What dressing should I use? How will this wound heal?’
An aspect of wound care management often overlooked is defining the wound itself. The guiding principles of wound care have always been focused around defining the wound, identifying any associated factors that may influence the healing process, then selecting the appropriate wound dressing or treatment device to meet the aim and aid the healing process.
This structured approach is essential, as the most common error in wound care management is rushing in to select the latest and greatest new wound dressings without actually giving thought to wound aetiology, tissue type and immediate aim.
This overview of wounds and dressings will identify some of the most common wound types and guide you in setting your aim of care and selecting a product or device to achieve that aim.
H.E.I.D.I. Holistic Assessment
The first thing to do before addressing any wound is to perform an overall assessment of the patient. An acronym used to guide this process, step by step, is H.E.I.D.I.:
- History
The patient’s medical, surgical, pharmacological and social history - Examination
Of the patient as a whole; then focus on the wound - Investigations
What bloods, x-rays, scans do you require to help you make your… - Diagnosis
- Implementation
Of the plan of care
So with this in mind and having completed a thorough overall assessment, the wound assessment can now be conducted.
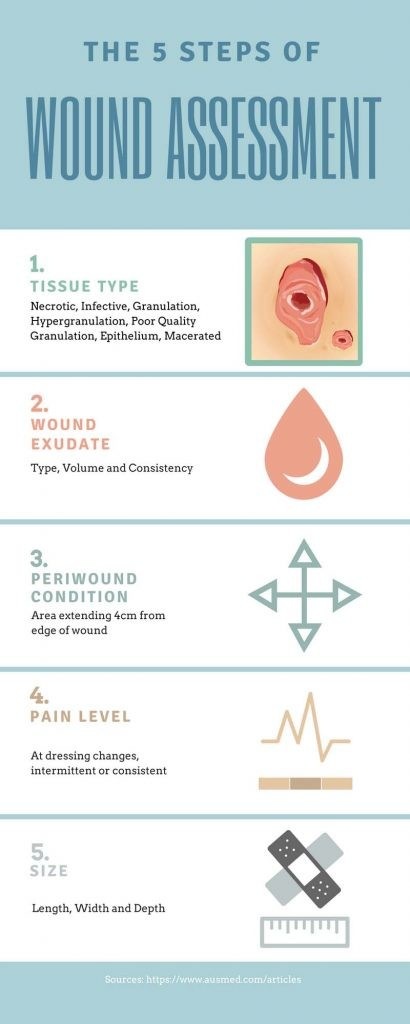
Wound Care Assessment Overview
The 5 parameters to consider in wound assessment include:
- Tissue type
- Wound exudate (type, volume and consistency)
- Periwound condition (this is the area that extends four centimetres from the edge of the wound)
- Pain level (at dressing changes, intermittently or consistently)
- Size (length, width and depth)
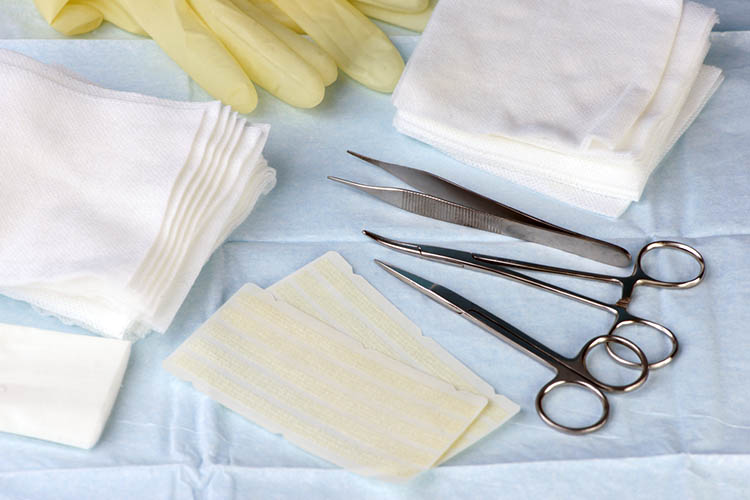
Dressing Surgical Wounds
Most surgical wounds go on to heal in the normal pathway of:
- Inflammation
- Proliferation (a very small process in healing sutured wound)
- Epithelialisation
- Maturation/contraction
Most surgery can be categorised into two groups: elective (‘clean‘) and emergency (this is often referred to as ‘dirty’). A surgical wound of the latter category has a higher incidence of dehiscence or complications.
Dehiscence is defined as ‘separation of the layers of a surgical wound, it may be partial or only superficial, or complete with separation of all layers and total disruption’ (Miller-Keane Encyclopedia and Dictionary of Medicine, Nursing, and Allied Health 2003).
There are a number of well-identified risk factors that can lead to wound dehiscence, including being overweight, increasing/advanced age, poor nutrition, diabetes, smoking and having had radiation therapy previously in the area. The elective case has the opportunity to correct some of these risk factors, however, the emergency case may not have such an opportunity.
Management
The simple, straightforward suture line is generally treated with a dressing that will manage a small amount of anticipated, early inflammatory exudate and provide a waterproof covering.
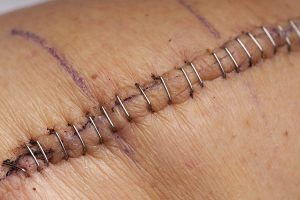
All surgical wounds do require support and this is an important factor both for reducing oedema and ensuring patient comfort. This type of dressing is generally left intact for five to seven days and then removed for inspection of the suture line, with the view to remove the staples or sutures as prescribed.
Suggested dressings to achieve the aims for simple suture lines include Opsite™ and Mepore Pro™. Care of this simple suture line then involves continued support and hydration. For this, some surgeons prefer supportive adhesive flexible tape for ongoing scar hydration, such as Fixomull™ and Mefix™.
The dehisced surgical wound requires a thorough assessment of cavities or structures involved, as well as the presence of foreign bodies, infection and/or necrotic tissue. Once these parameters have been considered, an aim can be set.
Removal of necrotic tissue and management of infection is paramount to move on to the wound-healing phase. Surgical debridement may leave large cavities or areas of raw tissue which can ideally be managed with a Topical Negative Pressure device. This wound care ‘vacuum cleaner’ will remove excess exudate and contain it in a canister, away from the wound surface. Due to the negative pressure, the wound edges are drawn in, helping to promptly reduce wound surface. This also reduces oedema, an important aspect to consider in all instances of wound care.