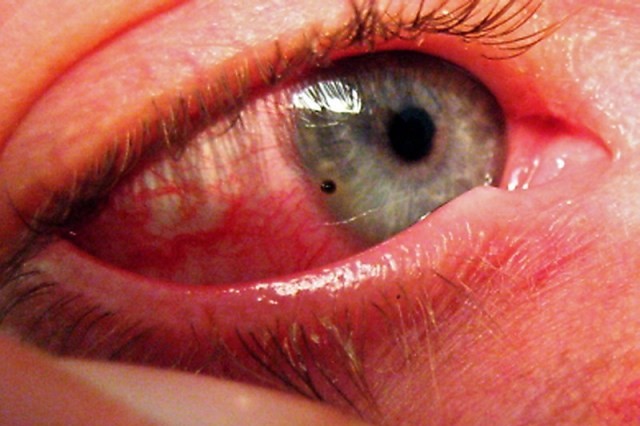
Corneal abrasions and foreign bodies in the eye: what to do? Diagnosis and treatment
Corneal abrasions are superficial, self-limiting epithelial defects. The most frequent conjunctival and corneal lesions are foreign bodies and abrasions
Improper contact lens wear can damage the cornea.
Although superficial foreign bodies often leave the cornea spontaneously in the tear film, sometimes they can leave a residual abrasion, other foreign bodies remain on or within the cornea.
Sometimes, a foreign body trapped below the upper eyelid causes one or more vertical corneal abrasions that worsen with blinking.
Cornial abrasions: can occur from apparently minor trauma
Intraocular penetration can occur in apparently minor traumas, particularly when foreign bodies come from high-speed tools (e.g., drills, saws, any tool with a metal-on-metal mechanism), from hammer use, or from blowouts.
With a corneal wound, infection does not usually develop from a foreign metal body.
However, corneal scarring and rust deposits can develop. In addition, if a corneal foreign body consists of organic material, an infection may develop.
If intraocular penetration is not recognised, regardless of the composition of the foreign body, an infection may develop within the eye (endophthalmitis).
Corneal abrasions and foreign bodies in the eye: symptoms
Symptoms and signs of corneal abrasion or foreign body presence include the sensation of the presence of a foreign body, tearing, redness and sometimes discharge.
Vision is rarely affected (unlike in the case of lacerations).
Diagnosis in cases of corneal abrasions and foreign bodies in the eye
- Slit-lamp examination, usually with fluorescein staining
After instilling an anaesthetic into the lower fornix (e.g. 2 drops of proparacaine 0.5%), each eyelid is inverted, and the entire conjunctiva and cornea are inspected with a binocular (magnifying) lens or slit lamp.
Fluorescein staining by illumination with cobalt light makes abrasions and non-metallic foreign bodies more obvious.
The Seidel sign is the flow of fluorescein from a corneal tear, which is visible during slit lamp examination.
A positive Seidel’s sign indicates a loss of aqueous humour through a corneal perforation.
Patients with multiple vertical linear abrasions should have their eyelids everted to search for a foreign body below the upper eyelid.
Patients with a high risk of intraocular injury or (more rarely) with a visible bulbar perforation or with a tear-shaped pupil undergo CT scan to exclude an intraocular foreign body and should be seen by an ophthalmologist as soon as possible.
MRI should not be prescribed if a metal foreign body is suspected because of the possibility of the metal moving and causing further injury.
Treatment of corneal abrasions and foreign bodies in the eye
- For superficial foreign bodies, irrigation or removal with a moist cotton bud or small needle
- For corneal abrasions, antibiotic ointment and pupil dilation
- For intraocular foreign bodies, surgical removal
After instilling an anaesthetic into the conjunctiva, doctors can remove conjunctival foreign bodies by irrigation or by removing them with a moist sterile cotton swab.
A corneal foreign body that cannot be removed by irrigation should be carefully removed with the tip of a sterile spatula (an instrument designed to remove ocular foreign bodies) or a 25- to 27-gauge hypodermic needle under magnification by binocular loupes or, preferably, by magnification with a slit lamp; the patient should be able to stare without moving the eye during removal.
Foreign bodies of steel or iron that remain on the cornea for more than a few hours may leave a rust ring on the cornea, which in turn must be removed under slit-lamp magnification by scraping or using a low-speed rotary bur; removal is usually performed by an ophthalmologist.
Abrasions
In most cases of corneal abrasion, an ophthalmic antibiotic ointment (e.g. bacitracin/polymyxin B or ciprofloxacin 0.3% 4 times/day for 3-5 days) should be prescribed until the epithelial defect has healed.
Contact lens wearers with corneal abrasions require an antibiotic with optimal anti-pseudomonas coverage (e.g. ciprofloxacin 0.3% ointment, 4 times/day).
For symptomatic relief of larger abrasions (e.g., with an area > 10 mm2), the pupil should also be dilated once with a short-acting cycloplegic (e.g., 1 drop of cyclopentolate 1% or homatropine 5%).
Eye patches may increase the risk of infection and are not usually used, particularly for abrasions caused by contact lenses or objects that may be contaminated by soil or vegetation.
Ophthalmic corticosteroids tend to promote fungal growth and reactivation of the herpes simplex virus and are contraindicated.
Continued use of topical anaesthetics may compromise healing and is therefore contraindicated.
Pain can be managed with oral analgesics.
The corneal epithelium regenerates rapidly; even extensive abrasions heal in 1-3 days.
Contact lenses should not be worn until the wound has healed.
A follow-up visit to an ophthalmologist 1-2 days after the injury is recommended, especially if the foreign body has been removed.
Intraocular foreign bodies
Intraocular foreign bodies require immediate surgical removal by an ophthalmologist.
Systemic and topical antimicrobials (effective against Bacillus cereus if the lesion is contaminated with soil or vegetation) are indicated; these include ceftazidime 1 g EV every 12 h, in combination with vancomycin 15 mg/kg EV every 12 h and moxifloxacin 0.5% ophthalmic solution every 1-2 h.
Ointments should be avoided if the eyeball is lacerated.
A protective cup (such as Fox’s cup or the lower third of a paper cup) is applied and hinged over the eye to prevent accidental pressure from causing the ocular contents to leak through the site of penetration.
Plasters should be avoided.
Tetanus prophylaxis is indicated after open eyeball injuries.
As with any laceration of the eyeball, vomiting (e.g. due to pain), which can increase intraocular pressure, should be avoided.
If nausea is present, an antiemetic may be prescribed.
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Autoimmune Diseases: The Sand In The Eyes Of Sjögren’s Syndrome
Blepharoptosis: Getting To Know Eyelid Drooping


