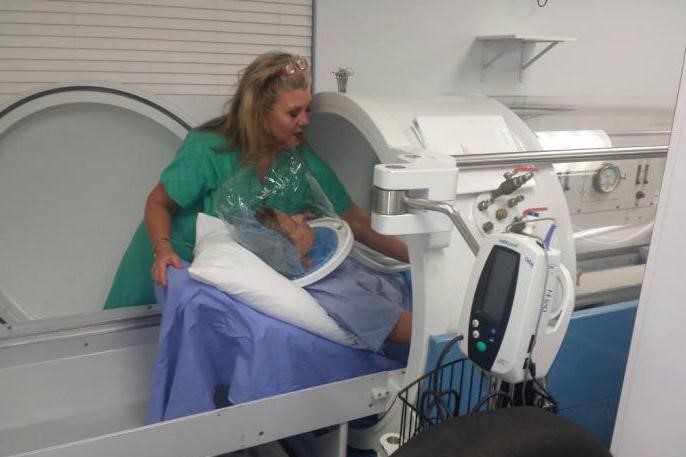
Decompression sickness: what it is and what it causes
Decompression sickness occurs when a rapid reduction in pressure (e.g. rapid surfacing, exiting a caisson or hyperbaric chamber, or ascending to high altitude) causes gases previously dissolved in blood or tissue to form bubbles within blood vessels
Symptoms typically include pain, neurological symptoms or both.
Severe cases can be fatal.
Diagnosis is clinical.
The definitive treatment is recompression therapy.
Correct diving techniques are essential for prevention.
Henry’s law states that the amount of gas dissolved in a liquid is directly proportional to the partial pressure of the gas in equilibrium with the liquid.
Thus, the amount of inert gases (e.g. nitrogen, helium) dissolved in blood and tissue increases as pressure increases.
During ascent, when the external pressure decreases, bubbles (mainly N2) may form.
Bubbles of free gas can form in any tissue and cause local symptoms or can be carried by blood to distant organs (arterial gas embolism).
Bubbles cause symptoms by
- Blockage of blood vessels
- Tissue rupture or compression
- Induction of endothelial damage and plasma extravasation
- Activation of coagulation and inflammatory cascades
Since nitrogen dissolves easily in adipose tissue, tissues with a high lipid content (e.g. central nervous system) are particularly susceptible.
Risk factors for decompression sickness
Decompression sickness occurs in about 2-4 dives/10 000 among recreational divers.
The incidence is higher among commercial divers, who are exposed to greater depths and longer dive times.
All of the following include risk factors:
- Low dive temperature
- Dehydration
- Exercise after diving
- Fatigue
- Flying after diving
- Obesity
- Advanced age
- Repeated or deep dives
- Rapid ascent
- Left/right heart shunts
Since excess nitrogen remains dissolved in the tissues for at least 12 h after each dive, repeated dives in the same day are more likely to cause decompression sickness.
Decompression sickness can also develop when the pressure drops below atmospheric pressure (e.g., with subsequent exposure to high altitudes).
Classification of decompression sickness
In general, two types of decompression sickness are distinguished:
Type 1: involves joints, skin and lymphatic vessels and is typically milder and not life-threatening
Type 2: includes neurological or cardiorespiratory involvement, which is severe, sometimes life-threatening and affects various systems.
The spinal cord is particularly vulnerable; other vulnerable areas include the brain, respiratory system (e.g. pulmonary emboli) and circulatory system (e.g. heart failure, cardiogenic shock).
The term The bends refers to local joint or muscle pain due to decompression sickness, but is often used as a synonym for any component of the syndrome.
General reference
Vann RD, Butler FK, Mitchell SJ, et al: Decompression illness. Lancet, 8;377(9760):153-64, 2011. PMID: 21215883. doi: 10.1016/S0140-6736(10)61085-9
Symptomatology of decompression sickness
Severe symptoms may occur within minutes of emergence, but in most patients symptoms begin gradually, sometimes with prodromes of malaise, exhaustion, lack of appetite and headache.
Symptoms occur within 1 h of emergence in about 50% of patients and within 6 h in 90% of cases.
Rarely, symptoms may occur 24-48 h after surfacing, particularly with exposure to high altitudes after diving (such as air travel).
Type I decompression sickness usually causes progressively worsening pain in joints (usually elbows and shoulders) and muscles; the pain usually does not intensify during movement and is described as ‘deep’ and ‘uncomfortable’.
Other manifestations include lymphoedema, tingling, itching and skin rash.
Type II decompression sickness consists of neurological and sometimes respiratory symptoms.
It typically manifests as paresis, paresthesias and tingling, dysuria and loss of voluntary control of bowel or bladder sphincters.
Headache and fatigue may be present, but are not specific complaints.
Lipotimia, tinnitus and hearing loss may occur if the inner ear is affected.
Severe symptoms include seizures, slurred speech, loss of visual acuity, confusion and coma.
Death may occur.
Chokes (respiratory decompression sickness) is a rare but serious manifestation; symptoms include wheezing, chest pain, coughing from pulmonary oedema.
Significant gas embolisation of the pulmonary vascular tree can lead to rapid circulatory collapse and death.
Dysbaric osteonecrosis is a late complication of decompression sickness, and often occurs without any previous symptoms.
It is an insidious form of osteonecrosis caused by prolonged or very close exposures to increased pressure (typically in people working in compressed air and in professional rather than recreational divers).
Deterioration of the articular surfaces of the shoulder and hip can result in chronic pain and disability due to secondary osteoarthritis.
Decompression sickness, diagnosis
The diagnosis is clinical.
CT and MRI scans may be useful to exclude other pathologies causing similar symptoms (e.g. herniated intervertebral disc, ischaemic stroke, central nervous system haemorrhage).
Although these tests sometimes reveal brain or spinal cord abnormalities due to decompression sickness, their sensitivity for decompression sickness is low and treatment should usually be undertaken on the basis of clinical suspicion.
Arterial gas embolism may have a similar manifestation.
However, immediate treatment for both is similar.
In the case of aseptic osteonecrosis, skeletal X-ray shows joint degeneration that cannot be distinguished from that caused by other joint diseases; MRI is usually diagnostic.
Treatment of decompression sickness
- 100% oxygen
- Recompression therapy
- Infusion therapy to maintain intravascular volume
Most patients recover completely.
Initially, high-flow 100% oxygen therapy facilitates nitrogen elimination by increasing the nitrogen pressure gradient between the lungs and circulation, thereby accelerating the reabsorption of nitrogen-containing gas emboli.
To restore lost intravascular volume, oral resuscitation fluid (or plain water) is indicated for patients under observation with mild manifestations.
Isotonic EV fluids without glucose are indicated for those with severe manifestations.
Recompression therapy is indicated for all patients; those with symptoms limited to pruritus, flaky skin and fatigue, which may be treatable with oxygen alone, are exempted; patients should be observed for possible worsening of symptoms.
Patients with more severe symptoms are transported to a suitable facility for recompression.
As the time interval before treatment and the severity of the injury are important determinants of prognosis, transport should not be delayed for non-essential procedures.
If air transport is necessary, cabin pressurisation of 1 atmosphere is highly recommended.
In unpressurised aircraft, preferably maintaining a low altitude (< 609 m [< 2000 ft]) and continuous oxygen supply.
Commercial aircraft, despite being pressurised, usually have cabin pressure of up to an equivalent of 2438 m at a normal cruising altitude, which can exacerbate symptoms.
Flying in commercial aircraft immediately after a dive may exacerbate symptoms.
Treatment refere nce
Moon RE, Mitchell S: Hyperbaric treatment for decompression sickness: current recommendations. Undersea Hyperb Med, 46(5):685-693, 2019. PMID: 31683368.
Prevention
Significant bubble formation can usually be prevented by limiting the depth and duration of dives to limits that do not require decompression stops during ascent (so-called no-stop limits) or by making ascent with decompression stops as indicated by guidelines (e.g., the decompression tables in the Diagnosis and Treatment of Decompression Illness chapter of the US Navy Diving Manual).
Many divers wear a handheld dive computer that continuously records depth and time spent at each depth and compiles a decompression profile.
In addition to following the published profiles and dive computer guidelines, many divers perform a safety stop for a few minutes at a depth of about 4.6 m from the surface.
However, cases may occur even after proper diving within the no-stop dive limits, or conversely, the incidence of decompression sickness does not decrease despite the widespread use of dive computers (although fewer severe cases occur).
Dives made < 24 hrs apart (repeated dives) require special technical measures to carry out correct decompression procedures.
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Emergency Rescue: Comparative Strategies To Exclude Pulmonary Embolism
Pneumothorax And Pneumomediastinum: Rescuing The Patient With Pulmonary Barotrauma
Barotrauma Of The Ear And Nose: What It Is And How To Diagnose It


