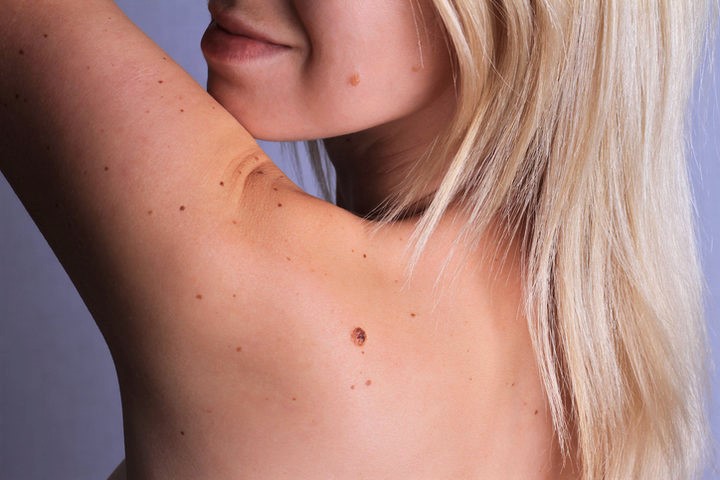
Dermatological examination for checking moles: when to do it
Moles (or nevi) are pigmented formations of the skin or mucous membranes resulting from an abnormal development of melanocytes, cells that are normally present in our skin
Usually, moles appear as circumscribed patches, roundish or oval in shape, flat or raised in relation to the surrounding skin.
Moles can vary in size and colour and can change over time
Some changes are harmless, while others, affecting for example shape and size, can be an alarm bell.
For this reason it is advisable to have regular check-ups with a dermatologist to detect melanomas when they are still in their early stages.
Nevi: what do benign tumours on our skin look like?
Knowing your moles is important: being informed is the first step towards effective prevention.
We must therefore know that our moles can vary in shape, size and colour.
A mole can be flat, slightly rounded or protrude noticeably from the skin, it can be of different sizes and colours ranging from dark pink to dark brown.
Approximately 30% of melanomas evolve from a pre-existing mole, while the remaining 70% develop “de novo”, i.e. in a place in the skin where no mole was previously present.
Although in the early stages it is still difficult to tell the difference between a nevus and a melanoma, during the dermatological examination the features that allow the specialist to highlight the presence of a malignant tumour, or a suspicious evolution, are already evident.
However, when a pigmented lesion grows or changes significantly, it is easy even for the patient to notice an alarm bell: in that case it is necessary to contact the specialist immediately.
Risk factors for moles
There are some well-known risk factors for the development of melanomas: people who have more than 100 moles, and people with a light phototype (blue/green eyes, fair skin, tendency to sunburn).
In any case, it is good for all patients, regardless of the presence of these risk factors, to know good practices to reduce the possibility of melanoma occurrence and the elements to take into account when checking their skin.
What are the risk factors of moles that are modifiable, i.e. not related to genetics and family history, for melanoma?
UV lamps are certainly a danger to our skin and should be avoided.
Direct sunlight is also to be avoided, so it is important to always use sunscreen with a high filter (SPF 50 or more) and to cover up during the hottest hours with sunglasses, hats and light but opaque clothing.
Sunburn and intense photo-exposure are therefore the main risk factors for the development of skin cancer, especially if these events occur early in life (childhood/adolescence).
Moles: signs not to be underestimated
In order to be able to control the changes that moles undergo over the years it is advisable to follow a regular course of prevention, which goes beyond the daily observation of one’s own skin.
The latter should be carried out in any case, taking into account the “ABCDE” mnemonic rule that allows a suspicious pigmented lesion to be identified and brought to the attention of the dermatologist, without waiting for the periodic check-up.
- asymmetry: more attention should be paid if a nevus is asymmetrical.
- edges: if irregular
- colour: pay attention to the number of colours of the lesion; the presence of more than one colour within the same “mole” should not be underestimated
- diameter: if greater than 6 mm
- evolution: if what appears to us to be a mole develops too quickly, we should consider it an alarm bell.
Moles check-up: an appointment with prevention
Learning to look at your body and check the condition of your moles is important, but this does not mean that you can do without regular visits to your dermatologist.
Once they reach adulthood, every individual should have a dermatological check-up once a year, especially in the case of patients with high risk factors (for whom a closer follow-up may be required by the specialist).
This is a special lens that allows the dermatologist to identify the presence of a melanoma or a highly atypical nevus before it is recognisable to the naked eye.
If recognised in its early stage, melanoma can be removed surgically with a simple outpatient procedure under local anaesthesia.
On the other hand, an advanced melanoma can represent a serious risk to the patient’s health, and can even develop metastatically.
If the specialist considers it necessary, in selected cases (patients with numerous lesions, deserving close monitoring) a second level examination, mole mapping, may be required.
This is an examination that allows the status of individual moles to be monitored by acquiring not only macroscopic but also dermoscopic images.
The examination consists of observing all the moles on the patient’s body, on both sides, using a computerised videodermatoscope, a lens instrument with an HD camera that, when placed on each mole, provides a detailed image of it.
At the end of the examination, the images are archived and then superimposed on those taken at subsequent examinations, so that any clinically significant changes or the appearance of a new lesion are evident.
What to do if a mole breaks?
A mole may break, perhaps as a result of trauma or abrupt rubbing.
Contrary to popular belief, a broken mole is no more likely to develop into a melanoma than a healthy one and is therefore no more dangerous than a normal mole.
However, a ruptured nevus should not be taken lightly: any over-infection of the wound may conceal the true appearance of the nevus, making it difficult to evaluate clinically and dermatoscopically.
In any case, a traumatised nevus should be evaluated by a dermatologist together with all the other moles, after the trauma has been resolved (applying an antibiotic cream if deemed necessary by the treating physician).
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Psoriasis, An Ageless Skin Disease
SkinNeutrAll®: Checkmate For Skin-Damaging And Flammable Substances
Healing Wounds And Perfusion Oximeter, New Skin-Like Sensor Can Map Blood-Oxygen Levels
Psoriasis, An Ageless Skin Disease
Epidermolysis Bullosa And Skin Cancers: Diagnosis And Treatment


