What is TTTS or Twin to Twin Transfusion Syndrome?
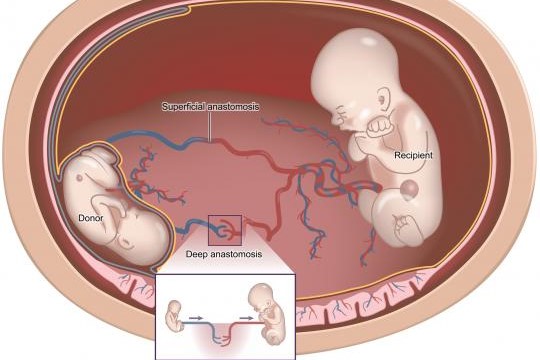
TTTS or Twin to Twin Transfusion Syndrome is an acute illness characteristic of twins who share a placenta and is characterised by the abnormal passage of blood from one twin (donor) to the other (recipient)
This imbalance leads to an increase in the volume of fluid in the recipient twin, resulting in an increase in the amount of urine emitted (polyuria).
Polyuria results in an excess of fluid in the amniotic sac (polydramnios).
On the other hand, in the donor twin’s sac there is a marked reduction in the amount of amniotic fluid until it is completely absent (anhydramnios) and circulatory changes due to the decrease in blood volume.
What are the causes of TTTS or Twin to Twin Transfusion Syndrome?
In all twin pregnancies with a single placenta there is an area of the placenta, called the vascular equator, where the placental blood vessels belonging to the territory of one twin enter into communication with the vessels belonging to the placental territory of the other twin, through the presence of connections (anastomoses) between the blood vessels.
When the balance between the twins’ blood vessels is disturbed, the disease occurs, but why this happens is not yet known.
How common is TTTS or Twin to Twin Transfusion Syndrome?
Approximately 10-15% of pregnancies with twins who share a placenta but are each enclosed in their own amniotic sac develop TTTS.
The disease is less frequent (4%) in pregnancies in which twins share both the placenta and the amniotic sac.
Diagnosis of TTTS or Twin to Twin Transfusion Syndrome
The diagnosis of fetal-to-fetal transfusion syndrome is by ultrasound. The basic prerequisite for the diagnosis, which is usually performed between 16 and 24 weeks, is the coexistence of abundant amniotic fluid or polydramnios of the recipient (maximum flap > 8 cm before 20 weeks and > 10 cm later) and reduced/absent amniotic fluid or oligohydramnios of the donor (maximum flap < 2 cm).
The evaluation of Doppler flowmetry of the umbilical cord and the ductus venosus in both fetuses also makes it possible to define the stage of evolution of the pathology.
Why do we intervene in cases of TTTS or Twin to Twin Transfusion Syndrome?
If left to their natural course, severe forms of feto-fetal transfusion lead to the loss of one or both twins in the vast majority of cases. Furthermore, in the case of death of only one twin, it is very common to find a severe reduction in blood volume in the surviving twin.
This phenomenon is associated, in about 30-50% of cases, with the development of brain damage – of varying degrees, from language or motor learning delay to severe neuromotor or cognitive impairment – due to reduced oxygenation of the brain caused by the reduced blood supply to the surviving twin.
Action is always taken when there are abnormalities in the blood flow to one or both twins.
However, there are also cases where intervention is only required if the amniotic fluid in the recipient twin is so high that there is a risk of losing the pregnancy or rupturing the membranes or giving birth prematurely.
How is it treated?
The treatment of first choice for feto-fetal transfusion syndrome is endoscopic laser coagulation of placental vascular anastomoses.
The rationale for this procedure is to interrupt the abnormal exchange of placental blood vessels and to re-establish adequate circulation for both twins.
The procedure involves the use of an endoscope (fetoscope) approximately 3 mm in diameter, which is inserted into the amniotic cavity of the recipient twin via the maternal transabdominal route and allows direct vision of the placental surface.
A very thin laser fibre is then inserted into the fetoscope to coagulate the vascular connections (anastomosis) and divide the placenta into two separate districts.
The operation is carried out under local anaesthesia and sedation in an in-patient setting.
The average stay in hospital is 2-3 days. Maternal risks are very rare and treatable.
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Breast Milk Stimulates Infants’ Covid-19 Defences: A Study In Jama


