Women scarred with acid: what should the rescuer do?
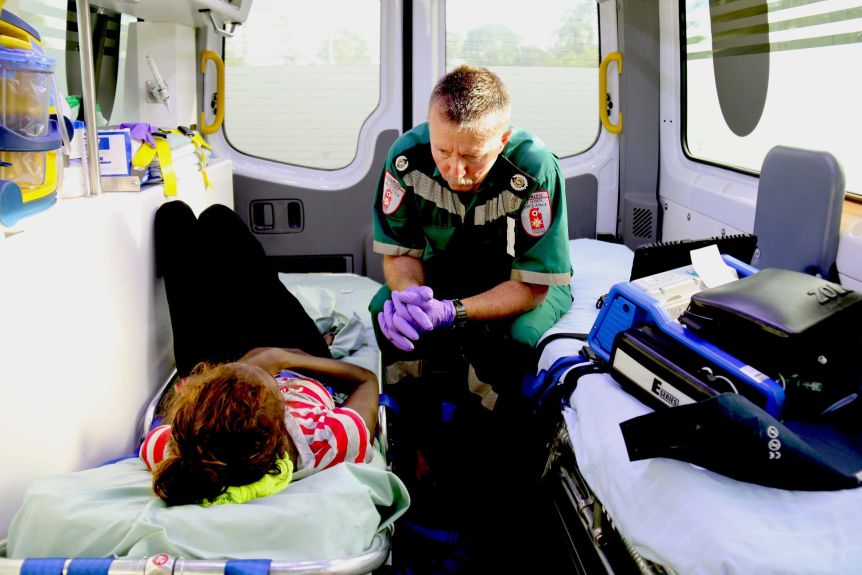
Acid attack: you need water, water and more water, and plenty of it. If you witness an acid attack, you have to intervene. This is what the first responder has to do.
Women scarred with acid: how should the rescuer or first responder act in the event of such serious assaults?
First of all, when you arrive at the scene, the first thing to assess is safety: how much acid is in the area, how serious the situation is, and whether the attacker is around, or whether there are any witnesses or people present who can help with the second thing to do, after assessing the severity of the burn.
That is, the possible search for an abundant source of water.
Many rescuers have a doubt: is water really the most appropriate compound to wash away the acid from such a wound?
The only answer is yes, with one caveat: in large quantities, because water is an amphoteric substance and to eliminate this characteristic, the quantity used for washing must be increased as much as possible.
It is no coincidence that on the boxes of acids and detergents, it is always indicated to wash any splashes of acid that end up on skin, eyes or clothes with running water.
Too little water would have the opposite of the desired effect.
ACID ATTACK AGAINST WOMEN, THE ANSWER IS IN THE WATER
Let’s see why:
– In chemistry, water is considered an amphoteric compound. That is, it behaves as a base with acids, and as an acid with bases. In balanced quantities (X acid and X water) the acid will act as a base and thus feed the chemical reaction of the acid, increasing its action.
So back to our case:
– If the person has been attacked with acid one must immediately wash the patient with running water or large quantities of water, continuously, until there is certainty that the acid has been completely washed away. The physiological saline in the ambulance is also fine (in fact, very fine). The important thing is to use a lot of it and not skimp on quantities.
– A tingling sensation in the throat or nose, or burning in the eyes, could be a sign of contagion from the chemical agent, which, when combined with water (but usually with little water), turns into gas and attacks the rescuer in another form. The area in contact with the acid – depending on the speed of intervention – will be more or less affected. Often, however, surgery is required to restore the affected part.
– Do not underestimate the severe physical pain the patient feels. In the initial phase the patient may be in shock, lose consciousness, lose control of the sphincters or have an epileptic fit. These symptoms are secondary to the action of the acid. The patient’s awakening is then a second critical phase: the pain experienced by the victim is severe and prolonged, with a strong burning sensation.
The victim of chemical burn oppure the chemical burned victim.
ACTIONS TO TAKE IN THE EVENT OF AN ACID ATTACK
It is advisable to remove any tissue that may have been soaked in the chemical.
If earrings, necklaces or piercings are present, they should not be touched (they will be removed at the hospital).
Once the affected area has been washed and once the emergency services and MSA have been called – or should the rescuers be voluteers be already on site- you can proceed with the search of the bottle used by the aggressor to hit the victim.
In this case, important information can be retrieved, such as the primary chemical agent, which can then be buffered by the doctor with the appropriate medicines and practices.
Remember that burns can be classified in different ways, because they are skin damage resulting from contact of the skin with corrosive agents, with agents that have temperatures higher than body temperature or with electric current (there are also burns from gamma rays and radiation).
The corrosive power of the agent, the time of exposure to the agent, the area of contact, and the age of the individual determine the severity of the burn.
Unfortunately liquid burns are more extensive than solid burns, although chemical powders that can cause damage, such as quicklime, should not be underestimated.
Burn damage is easily visible: it is an inflammatory reaction with vasodilatation and increased permeability of the epidermis, with leakage of plasma, followed by thrombosis of the dermal vessels, coagulative necrosis and – in severe cases – necrosis of the dermis and subcutis.
Women scarred with acid: the importance of the ‘rule of 9’.
 The burn must always be assessed and – irrespective of the cause – the depth, extent and site affected must be considered. A simple rule, the ‘rule of 9’, should be used to assess burns.
The burn must always be assessed and – irrespective of the cause – the depth, extent and site affected must be considered. A simple rule, the ‘rule of 9’, should be used to assess burns.
- Head and neck % 9
- Chest and abdomen % 18
- Posterior trunk and buttocks % 18
- Upper right limb %9
- Upper left limb % 9
- Lower right limb % 9
- Lower left limb % 9
- Genitals % 1
This is not the case for children, where the percentages increase because the body size is smaller.
RESCUING ATTACKED WOMEN: ASSAULT WITH ACID, BRIEF SUMMARY
So, in summary, once you arrive on the scene you should take
- General precautions: staff treating burn patients may be at risk of contracting infections (HIV, hepatitis C and B), and should therefore use PPE
- Immediately stop the burn process, remove clothing from the affected area, wash all areas thoroughly that have come into contact with chemicals, cut off the power flow in case of electrical injuries. This is where the activity allowed to the volunteer stops.
- Hydroelectric resuscitation. The nurse or doctor uses the universally used formula for the first 24 hours post-burn in adults is: 2-4 ml of ringer lactate x the body weight in kg x the % of body surface area burnt. 50% in the first 8 hours and the remainder in the next 16 hours.
- Vital parameters, to be assessed as often as necessary
- Placement of nasogastric tube, burns > 20% result in paralytic ileus with gastric dilatation
- Placement of bladder catheter with thermistor
- Assessment of extremity perfusion, ischaemia due to oedema below the eschar with risk of compartment syndrome
- Continuous assessment of respiratory activity
- Pain management and psychosocial assessment
The source of this chart is here and it was written by Dr Shpetim Daca, since 2012 contract professor at the University of Milan, nursing section.
assistenza alla persona ustionataRead Also:
Health In Swaziland, Women Risk Cancer For The Spread Of Clandestine Contraceptives
Rural Ambulances Fees Introduction, How Did They Impact On Pregnant Women Deliveries In Tanzania?