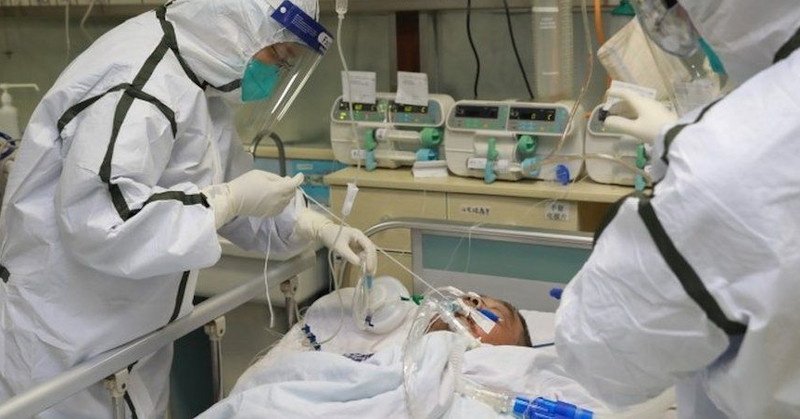
Risk of Parkinson's disease after COVID-19: an Australia a research
Parkinson’s disease. COVID-19 leaves deep scars in patients who have suffered from it. And not only to the respiratory system: also the nervous system is often affected by the damage caused by the coronavirus. All these “traumas” are now known as “post-COVID-19 syndrome”.
What’s up with Parkinson’s disease risk after surviving COVID-19. A research from Australia.
COVID-19 and Parkinson’s disease
Among the most evident signs of the post-COVID-19 syndrome is lack of energy, breathing difficulties, loss of memory and, in general, a more or less marked mental confusion. Less frequent are ageusia (loss of taste), anosmia (loss of smell) and skin rash. On the manifestations of the post-COVID-19 syndrome are overlapping studies around the world.
And this is a good thing: an early knowledge of the potential damage will lead to timely and more effective treatment of the coronavirus patient.
From Australia arrives a strong warning from the well-known Australian Institute of Neuroscience and Mental Health, the Florey, about the potential Parkinson’s disease risk of patients surviving COVID-19.
In the Journal of Parkinson’s Disease, Leah Beauchamp and the researchers she guides have published a scientific article that speaks explicitly about the brain’s degenerative consequences for patients.
A problem is so serious that they define this post-COVID-19 syndrome factor as “the third wave of the COVID-19 pandemic”, affecting brain damage three out of four patients. Damage ranging from loss of sense of smell to encephalitis.
Parkinson’s disease risk for three out of four COVID-19 patients: necessary mass screening for risk subjects
From this finding, on patients in Australia (but they are human beings biologically identical to Italians, so great attention must be paid while keeping alive the distinctions of coronavirus strain), the strong recommendation for a mass screening protocol that aims to identify people at risk of Parkinson’s disease.
They can then be treated with appropriate pharmacological therapies, able to slow down or stop the evolution of the disease.
“We need to change the community’s thinking that Parkinson’s disease is not a disease of old age. As we have heard over and over again, the coronavirus does not discriminate, and neither doesParkinson’s,” said Professor Kevin Barnham, Florey Institute of Neuroscience & Mental Health.
“We can understand the neurological consequences that followed the Spanish flu pandemic in 1918, where the risk of developing Parkinson’s disease increased two to three times.
Given that the world’s population was again affected by a viral pandemic, it is indeed very worrying to consider the potential global increase in neurological diseases that could develop along the way.
BELOW THE FULL STUDY
parkinson covid-19READ THE ITALIAN ARTICLE

