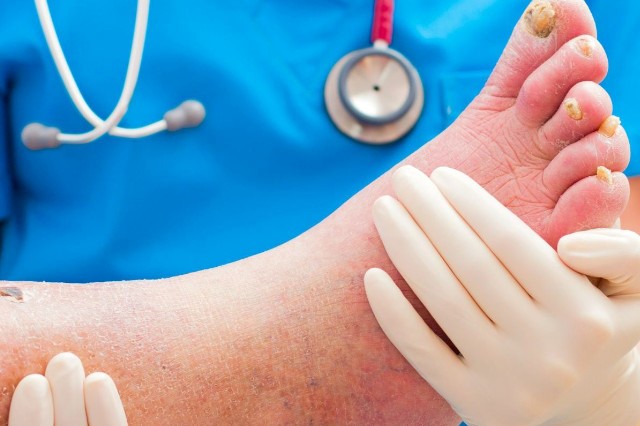
Diabetes mellitus: symptoms, causes and significance of the diabetic foot
The diabetic foot is one of the most dreaded complications of diabetes mellitus, a condition from which more than 1 million people worldwide lose a leg every year
The so-called diabetic foot is still an important and often disabling problem: a diabetic person has a relative risk of limb amputation 40 times higher than a non-diabetic person.
Early diagnosis and treatment are of paramount importance to avoid the worst consequences such as limb amputation.
Diabetic foot: what it is and what it causes
Diabetic foot refers to a chronic complication of diabetes mellitus, which causes anatomo-functional changes in the foot and ankle.
This condition is the result of several diseases that typically complicate diabetes mellitus, which is the most widespread form of diabetes and is also partly linked to lifestyle.
A condition whereby the body does not produce enough insulin or does not respond normally to insulin, causing excessively high levels of sugar (glucose) in the blood.
In particular, we speak of:
- motor and sensory neuropathies
- microcirculatory dysfunction;
- extreme vulnerability to infection;
- macroangiopathy, i.e. an alteration of the large blood vessels that favours the early appearance of atherosclerosis.
In fact, there is a close link between diabetic disease and the development of chronic micro- and macro-vascular complications.
This is due to the fact that excess blood sugar can facilitate the onset of atherosclerosis, i.e. the accumulation of fat in the walls of the arteries, which is responsible for the narrowing of large and medium-sized blood vessels.
Atherosclerosis in turn is a risk factor for:
- fatal and non-fatal coronary events, for which various epidemiological studies report a 1.5 to 3-4 times higher incidence in diabetics than in non-diabetics of the same age;
- other dreaded vascular complications due to a lack of or reduced oxygenation of tissues.
These include in particular:
- cerebral ischaemic events that may be transient or stable (TIA, stroke), when the carotid arteries are involved;
- arteriopathy obliterans of the lower limbs which may manifest itself with more or less disabling symptoms from claudication, i.e. pain when walking, to actual limb ischaemia. All these complications affecting the foot are called diabetic foot.
Symptoms of diabetic foot
The diabetic foot can present itself with a wide spectrum of infection ranging from superficial ulcerations to extensive gangrene of the foot.
Symptoms may include:
- increased temperature of the foot;
- lack of sensitivity to thermal, tactile and painful stimuli in the lower limbs;
- tingling;
- presence of scratches, cuts or skin ulcers.
The biggest problem in diabetic patients is the formation of skin lesions, even small ones, which can degenerate into ulcers and infections.
This is due to microcirculatory dysfunctions associated with peripheral arteriopathy: the feet do not receive an adequate supply of blood and oxygen, and they struggle more with the damage to the skin.
In addition, the skin of the diabetic foot becomes thinner and more fragile and therefore more vulnerable and exposed to infections, which represent one of the most serious threats since, if not assessed and treated promptly, they can lead to the need to amputate the affected foot.
It almost always happens that leg and foot injuries appear without warning and also worsen very quickly.
It is therefore essential that diabetes sufferers undergo regular preventive lower-limb check-ups to avoid the risk of worsening.
Since it is a disease that is very likely to lead to vascular complications, careful screening for vascular diseases of the various body districts is also essential.
Treatment of the diabetic foot: customised according to case and severity
The treatment of the diabetic foot depends on severity.
In addition to pharmacological control of diabetes, in general, in order to prevent the vascular complications of diabetes, it is essential to carefully monitor the vascularisation of the lower limbs and supra-aortic trunks.
This is also indispensable in people with little or no symptoms.
In the event of infection, treatment includes
- targeted antibiotic therapy, as indicated by the specialist, taking into account the pathogen responsible for the infection;
- in some cases, surgery.
In the case of complications affecting the lower limbs, so-called surgical revascularisation can be considered, which can be performed with traditional or minimally invasive endovascular surgery: the indication for one or the other technique derives from a careful objective examination of the patient together with non-invasive vascular diagnostics.
Today, the improved knowledge of atherosclerotic pathology of the lower limbs in these patients has opened up new frontiers in the field of peripheral revascularisation.
In the diabetic patient, atherosclerotic lesions have a very particular distribution, mainly involving the tibial arteries and the peroneal artery.
These are very small arteries and therefore difficult to approach with an ‘open’ surgical approach, which is why endovascular techniques have found an excellent field of application.
However, there are still many cases in which traditional surgery has a wide indication and cases in which a ‘hybrid’ approach with the simultaneous use of both techniques is recommended.
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Covid, Type 1 Diabetes Increasing Among Cured Minors
Type 2 Diabetes: New Drugs For A Personalised Treatment Approach
The Diabetic Diet: 3 False Myths To Dispel
Paediatrics, Diabetic Ketoacidosis: A Recent PECARN Study Sheds New Light On The Condition
Orthopaedics: What Is Hammer Toe?
Hollow Foot: What It Is And How To Recognise It
Occupational (And Non-Occupational) Diseases: Shock Waves For The Treatment Of Plantar Fasciitis
Flat Feet In Children: How To Recognise Them And What To Do About It
Swollen Feet, A Trivial Symptom? No, And Here’s What Serious Diseases They May Be Associated With
Varicose Veins: What Are Elastic Compression Stockings For?


