Eisenmenger syndrome: prevalence, causes, symptoms, signs, diagnosis, treatment, sporting activities
Eisenmenger syndrome is a set of symptoms and signs caused by a rare and complex association of cardiovascular abnormalities leading to pulmonary hypertension with bidirectional or reverse shunt with intracardiac or aorto-pulmonary communication
Eisenmenger syndrome often leads to sudden death
Historical background
Eisenmenger’s syndrome is named after Victor Eisenmenger, who first described it in 1897.
In 1958 Paul Wood was the first to use the term ‘Eisenmenger’s complex’.
Diffusion
Prevalence is 1-9/10000.
Age of onset
Eisenmenger’s syndrome usually develops before puberty, but can also occur in adolescence or early adulthood.
It begins after the age of two, on average around the age of fourteen.
It affects both males and females.
ECG EQUIPMENT AND DEFIBRILLATORS? VISIT THE ZOLL BOOTH AT EMERGENCY EXPO
Causes
Eisenmenger’s syndrome is due to the communication between the two cardiac chambers, as a result of a congenital defect or a surgically created shunt, which allows oxygenated blood to recirculate back into the right ventricle and into the lungs.
Over time, an increase in pulmonary resistance may develop, eventually leading to severe pulmonary hypertension, a bidirectional shunt with a progressively increasing right-left shunt.
Cardiac malformations leading to Eisenmenger syndrome
An interventricular septal defect (present singly or in tetralogy of Fallot or pentalogy of Fallot), if left untreated, can lead to the development of the syndrome.
Other cardiac defects that can lead, if untreated, to Eisenmenger’s syndrome are:
- pervious ductus arteriosus;
- aorto-pulmonary window;
- atrial septal defect;
- partial anomalous venous return (some pulmonary veins connect to the right atrium instead of the left atrium);
- truncus arteriosus.
Risk factors
Infants who have a large ventricular septal defect, atrial septal defect or persistent patent ductus arteriosus at birth have a higher risk of developing Eisenmenger’s syndrome.
Prevention
Eisenmenger’s syndrome can be prevented by corrective surgery before changes occur in the lungs.
Symptoms and signs of Eisenmenger’s syndrome
Clinical symptoms of the syndrome include:
- lack of air (especially during exercise),
- fatigue,
- lethargy,
- dizziness,
- cyanosis (bluish colour of the skin),
- syncope,
- hepatomegaly,
- peripheral oedemas,
- distension of neck veins,
- chest pain,
- palpitations,
- atrial and ventricular arrhythmias.
The left-right shunt due to Eisenmenger’s syndrome is responsible for systemic oxygen desaturation leading to:
- haemoptysis (later sign),
- secondary polycythaemia,
- hyperviscosity, haemoptysis,
- central nervous system events (such as cerebral abscesses or strokes),
- pulmonary artery thrombosis,
- sequelae of increased red blood cell turnover, such as
- hyperuricemia causing gout
- hyperbilirubinemia causing cholelithiasis,
- iron deficiency with or without anaemia.
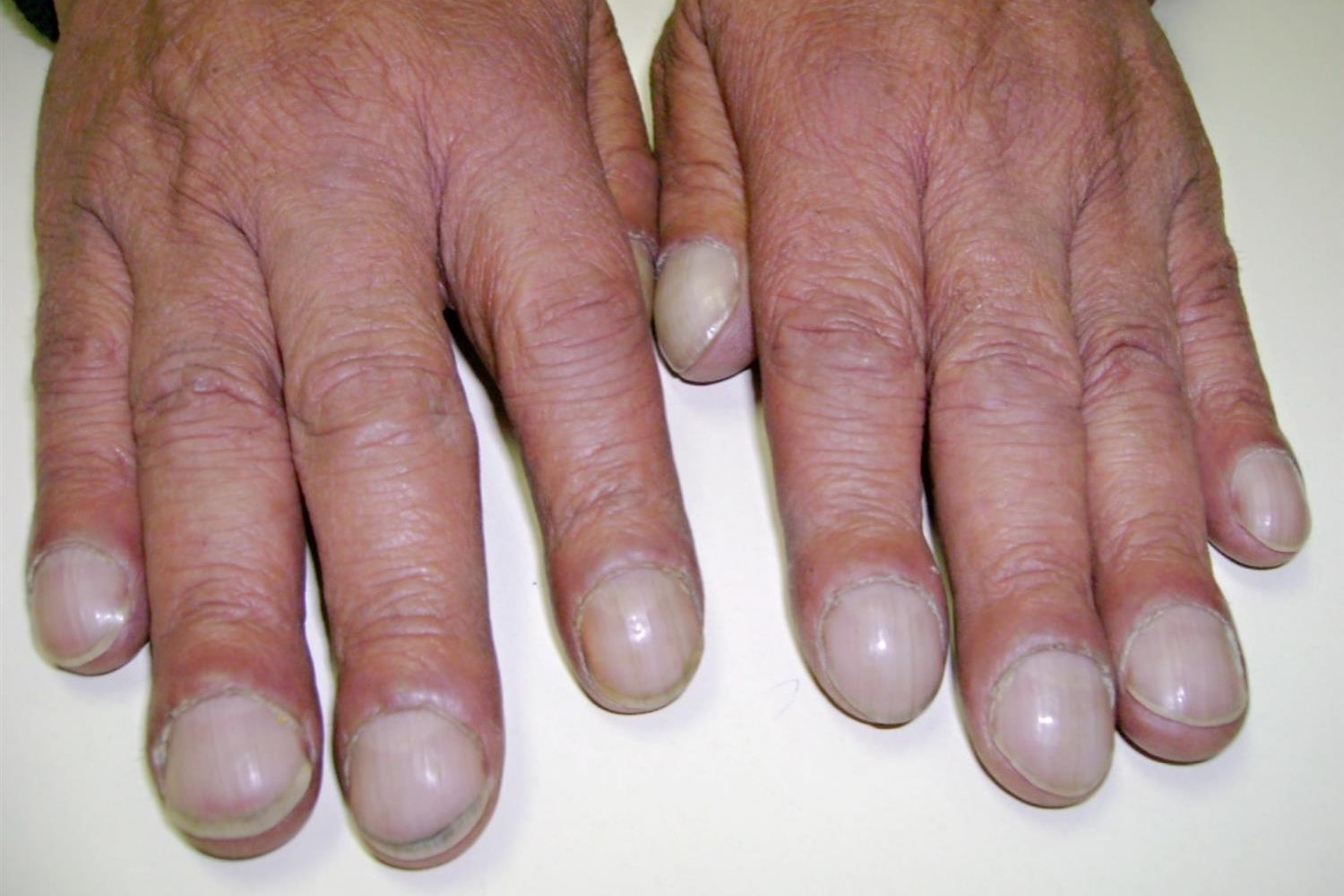
Digital hippocratism (“drumstick fingers”, see image below) and heart murmurs may be present.
- cerebral embolisms,
- endocarditis,
- right heart failure (associated with hepatomegaly, peripheral oedema, distension of the jugular veins),
- sudden death.
Secondary polycythaemia usually causes the following symptoms and signs:
- transient ischaemic attack with slurred speech,
- visual problems,
- headache,
- increased fatigue,
- signs of thromboembolism.
Abdominal pain may result from cholelithiasis.
Painful gouty arthritis may result from hyperuricemia.
Patients are at high risk of morbidity and mortality at delivery.
Diagnosis
The diagnosis of Eisenmenger’s syndrome is based on the clinical picture, electrocardiogram abnormalities and imaging.
On physical examination, central cyanosis and digital hippocratism are noted.
Signs of right ventricular decompensation (such as hepatomegaly, peripheral oedema, distension of neck veins) are often noted.
Palpation reveals a right ventricular quiver.
On auscultation, a holosystolic murmur from tricuspid insufficiency may be heard at the lower left sternal border; a sharp decreasing protodiastolic murmur from pulmonary insufficiency may also be heard along the left sternal border.
A strong, single second heart tone (S2) is a constant finding, and a pulmonary ejection click is frequent.
The diagnosis is confirmed by electrocardiogram, echocardiography with colordoppler, chest X-ray, cardiac catheterization and measurement of pulmonary artery pressure.
Laboratory tests
In patients with Eisenmenger’s syndrome, laboratory tests show polycythaemia with a haematocrit > 55%.
Increased erythrocyte turnover may reflect a condition of iron deficiency (e.g. thalassaemia), hyperuricaemia and hyperbilirubinaemia.
Iron deficiency may be related to iron deficiency anaemia and can be identified by measuring transferrin saturation and ferritin.
Electrocardiogram
In the patient with Eisenmenger syndrome, the electrocardiogram shows:
- right ventricular hypertrophy,
- right axial deviation,
- occasional right atrial dilatation and hypertrophy.
Chest X-ray
In the patient with Eisenmenger’s syndrome, the chest X-ray shows:
- prominent central pulmonary arteries,
- amputation of pulmonary vascular endings,
- enlargement of the right heart.
Therapy
There is no specific therapy that can cure the syndrome: the main focus of care for patients with Eisenmenger syndrome is to avoid conditions that may aggravate the syndrome, such as pregnancy, reduced circulating volume, isometric exercises, cigarette smoking or high-altitude activities.
Supplemental oxygen may provide some benefit. Surgery is generally contraindicated, and in adults, only heart and lung transplants are possible.
However, drugs capable of reducing pulmonary arterial pressure have been shown to at least slightly increase the chance of survival.
Prostacyclin analogues (treprostinil, epoprostenol…), endothelin antagonists (bosentan) and phosphodiesterase-5 inhibitors (sildenafil, tadalafil…) improve performance in the 6-minute walk test and reduce the N-terminal segment of brain natriuretic pro-peptide.
Aggressive therapy with pulmonary vasodilator drugs resulted – in a small number of patients – in a clear left-to-right shunt, allowing surgical repair of the underlying heart defect and a significant reduction in mean pulmonary artery pressure.
Prophylaxis for endocarditis prior to dental treatment or surgical procedures that are prone to cause bacteremia is useful.
Symptomatic polycythaemia can be treated with cautious bloodletting until the haematocrit has been lowered from 65% to 55% while volume is replenished with saline.
Compensated, asymptomatic polycythaemia, however, does not require bloodletting, regardless of the haematocrit.
Hyperuricaemia can be managed with allopurinol 300 mg orally once a day.
Preventive anticoagulant therapy is controversial because the risk of pulmonary artery thrombosis and other thromboembolic phenomena must be balanced against the risk of pulmonary haemorrhage.
Heart transplantation and lung transplantation can increase life expectancy, but are reserved for patients with severe symptoms and unacceptable quality of life.
Sporting activity
Patients with Eisenmenger’s syndrome should avoid sporting competitions and all athletic activities of a certain level of effort, especially at high altitudes, such as skiing.
Prognosis of Eisenmenger syndrome
The syndrome can be avoided by surgically correcting the anomalies before they lead to pulmonary changes; unfortunately, if the defects are not corrected in time, the syndrome develops and the prognosis gets much worse.
Life expectancy depends on the type and severity of the defect and right ventricular function, and on average varies between 20 and 50 years.
Risk factors that can worsen the prognosis are:
- haemorrhages,
- fever,
- vomiting,
- diarrhoea,
- pregnancy,
- puerperium,
- obesity,
- cigarette smoking,
- strenuous sporting activity,
- living at high altitudes,
- living in heavily polluted environments.
Mortality
The fetal mortality rate in pregnant patients with Eisenmenger syndrome is about 25%.
The maternal mortality rate exceeds 50%, which means that half of all women with Eisenmenger syndrome die during pregnancy.
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Emergency Data Management: ZOLL® Online Europe, A New European Cloud-Based Platform To Be Discovered
Paediatrics, New Ablation Technique For Tachycardia At The Bambino Gesù In Rome
Tachycardia: Important Things To Keep In Mind For Treatment
What Is Ablation Of Re-Entry Tachycardias?
Atrial Fibrillation Ablation: What It Is And How To Treat It
Treating Atrial Fibrillation With Percutaneous Closure Of The Left Auricle
Atrial Fibrillation: What It Is And How To Treat It