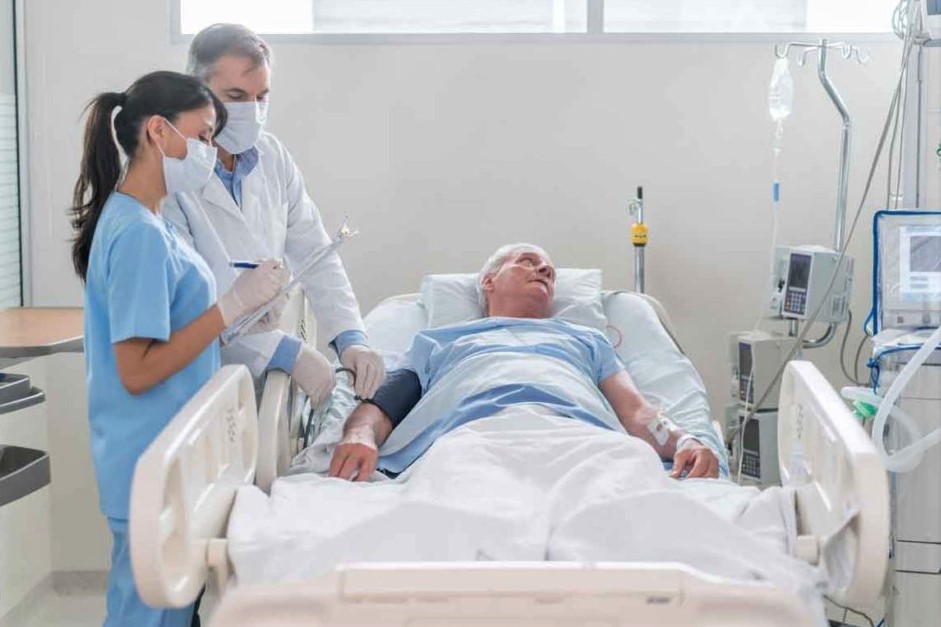
Post-intensive care syndrome (PICS): what is it?
Let’s talk about post-intensive care syndrome (PICS): perhaps never before has there been so much talk about intensive care as during this pandemic. We have become accustomed to the evening ‘bulletin’ of infections and admissions to ordinary wards and intensive care units
And those who are ill, hospitalised, become part of a figure, part of a group; the group of those who spend a period of their lives in an ‘ordinary ward’ or the group of those who, unfortunately, are seriously ill in intensive care.
However, there is another group, another figure that unfortunately nobody talks about.
It is a group of silent people who, having come out of intensive care (covid or no covid), have returned home and are trying to get their lives back on track.
Yes, because, as few people in Italy know and even less talk about, after a long stay in intensive care you still need intensive care.
We are talking about PICS, the post intensive care syndrome
A term coined by the Society of Critical Care Medicine in 2010 to identify those “impairments” caused precisely by admission to intensive care.
These are a bit like the side effects of drugs, those unintended effects, almost always negative, that flank the positive effects of the active ingredient.
The problem is that the effects of prolonged hospitalisation in intensive care are so great an impact on a person’s life (and that of their family) that recovery requires a great deal of effort.
Intensive care often requires long periods of sedation, where the person is immobile in bed (every two or three hours the ICU nurses change position if they can), breathing on an artificial ventilator, being fed artificially by tube, often requiring intravenous fluids, receiving antibiotics, anti-inflammatory drugs.
And one could go on and on, citing various ‘additional machines’ to which the patient is connected via catheters or cannulae.
When the covid pneumonia (or other pathology that caused the admission to the ICU) is finally defeated, after perhaps three or four weeks, the person will leave the ICU.
They will be biologically healed (or almost), even if other problems often start to emerge: psychological, cognitive, physical disorders that are grouped together under the name of post-intensive care syndrome.
Often people who leave intensive care begin to experience anxiety, even severe depression or even develop post-traumatic stress syndrome.
Sometimes they have memory problems, difficulty in concentrating, lack of appetite, muscular deficits.
PICS is hardly ever recognised and treated
Professionals themselves know very little about it and the most diligent doctors intervene by treating individual problems separately.
What is lacking is a “director’s office” capable of intervening simultaneously on several fronts, evaluating each situation as a whole, intervening not only on the patient but also on the family, which very often finds itself having to take on the role of care giver without having the knowledge and skills to deal with the problem.
This is why the post-intensive care portal postintensiva.it was created by a group of intensive care nurses who realised how little information (for families) and training (for health professionals) there is on post-intensive care syndrome.
Post-intensive care wants to inform families, train and try to create a network of professionals who can take care of the patient leaving the ICU.
Another very important aspect is the humanisation of the intensive care unit: strategies to improve the outcome and reduce the incidence of post-intensive care syndrome must be implemented during admission.
Post-intensive care promotes, for example, the ICU patient diary to reduce the psychological effects of hospitalisation.
This tool allows the patient to reconstruct what happened, to become aware and to face the convalescence period in a more serene way.
The humanisation of intensive care must also necessarily pass through models which place the patient and his family at the centre.
This is why post-intensive care promotes the model of open intensive care where family members can stay close to their loved ones during one of the hardest moments of life.
Postintensive care is always looking for nurses, health workers, patients’ families or former patients who want to collaborate in spreading an idea of humanisation that we hope will take root more and more in our hospitals.
Article written by Sergio Calzari
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
When Drunken Bystanders Don’t Want To Collaborate With EMS – The Difficult Treatment Of A Patient
Post-Intensive Care Syndrome (PICS) And PTSD In COVID-19 Patients: A New Battle Has Begun


