Venous thrombosis: from symptoms to new drugs
Venous thrombosis is a disease caused by the formation of a blood clot within the venous system
The formation of a blood clot is a physiological process that occurs whenever the body needs to stop a haemorrhage; however, there are situations in which the formation of a blood clot occurs in the veins in an inappropriate manner and in inappropriate locations and this can lead to venous thrombosis, a very serious disease that causes obstruction to the reflux of blood within our veins.
The causes of venous thrombosis
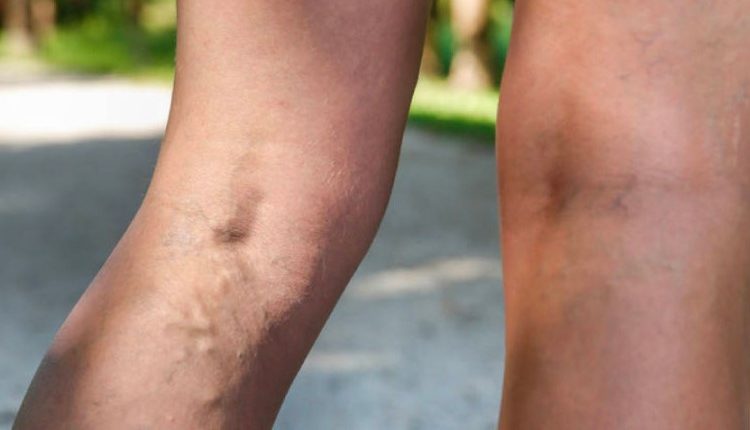
One of the causes is stasis, or the tendency of the blood to stagnate in the distal parts of our body, a condition that can be linked to varicose veins or to a period of bedding or significant limitation of mobility.
However, the main cause is inflammation: all chronic or acute inflammatory diseases, including pneumonia for example, cause the blood to clot more.
Other important risk factors are obesity, the presence of a tumour (in these patients, thrombosis often develops before the tumour itself), and estroprogestin hormone contraceptive or substitutive therapies after the menopause, which, however, represent a risk factor especially in those who are predisposed, for example those who have a significant family history of venous thrombosis”.
Venous thrombosis, the signs not to underestimate
Venous thrombosis is a very insidious disease whose symptoms can be very variable.
Generally speaking, the most affected organs (every vein in the body can have a thrombosis, including cerebral veins) are the lower limbs and the most classic symptoms are an increase in volume and swelling that may be limited to the foot or may extend to the calf or the whole leg.
There may also be barely perceptible to unbearable pain and a strong sense of heaviness in the leg, which may limit or even prevent limb movement or walking.
Compression ultrasound for the diagnosis of venous thrombosis
The clinical diagnosis of deep vein thrombosis is flawed and therefore it is essential to confirm the diagnosis by performing a safe, quick and painless ultrasound examination.
Vascular probe echocolordoppler is used in its simplest but most effective variant, compression ultrasound (CUS).
The veins of the legs are visualised, starting from the groin region, based on the principle that veins – unlike arteries – are compressible and therefore if a vein has a normal flow and does not have a thrombus, when pressed with the probe it compresses completely and is practically no longer visible on the monitor.
The entire length of the vein must be investigated because the thrombus may only be present in part of its course, and if we limit ourselves to exploring only the most proximal parts, which are easier to investigate, we risk not making a diagnosis and therefore not treating a potentially fatal pathology.
If the veins are compressible, the blood flows through them naturally and therefore there are no thrombi.
It is always a good idea to undergo this examination as a matter of urgency in the presence of a clinical suspicion of deep vein thrombosis, when all or even some of the symptoms described above appear and especially if they are associated with the presence of important risk factors.
What are the complications?
The most feared complication is pulmonary embolism, an infarction of the lung that leads to a significant impairment of respiratory function.
The veins of the lower limbs flow into the vena cava at abdominal level, which flows into the right heart from where the pulmonary arteries, which carry blood to the lungs, start.
A clot that forms in the veins of our legs, if not treated promptly, can break up into emboli and following the flow of blood from the periphery towards the heart, the emboli can reach the heart and from there into the lungs, where they occlude the pulmonary arteries.
Thus, a venous pathology is complicated by an arterial thrombosis, in which a vessel carrying blood to an organ is occluded, resulting in the death of the organ or part of it, with a more or less extensive infarction.
New treatments for venous thrombosis
Only anticoagulant drugs should be used to treat venous thrombosis; for about seventy years we had only one drug available that was very effective but complicated to manage, coumadin.
In the last 5-10 years, however, new drugs have become available, called new direct anticoagulants (NAO or DOAC), which have represented a real revolution in the field of therapy and prevention of both venous and arterial thrombosis (e.g. cerebral stroke in patients with atrial fibrillation, a frequent arrhythmia of the heart).
These drugs are easier to manage and safer; they are direct inhibitors of a single clotting factor and therefore do not require any monitoring other than periodic blood checks, sometimes only annually.
Read Also:
COVID-19, The Mechanism Of Arterial Thrombus Formation Discovered: The Study
The Incidence Of Deep Vein Thrombosis (DVT) In Patients With MIDLINE
Deep Vein Thrombosis Of The Upper Limbs: How To Deal With A Patient With Paget-Schroetter Syndrome
Knowing Thrombosis To Intervene On The Blood Clot
Venous Thrombosis: What It Is, How To Treat It And How To Prevent It


