What is Lyme disease and what are its symptoms?
Lyme disease is a tick-borne illness. How does it manifest itself? Let’s go into more detail with the specialist
Lyme is a city in the United States of America where in 1975 the first case of what has been called ‘Lyme disease’ was detected.
What is Lyme disease?
Lyme disease or Lyme borreliosis is a multisystem disease (affecting different organs and parts of the body), caused by a bacterium: Borrelia, a spirochaete that is transmitted to humans through the bite of an infected tick.
Symptoms of Lyme disease
As it is a multisystem disease, the symptoms can be extremely varied and differ depending on the stage of the disease.
In terms of disease manifestations, the disease has 3 different ‘stages’.
Stage 1: erythema migrans and Borrelia lymphocytoma
From a dermatological point of view, the initial phase of the disease can be characterised by
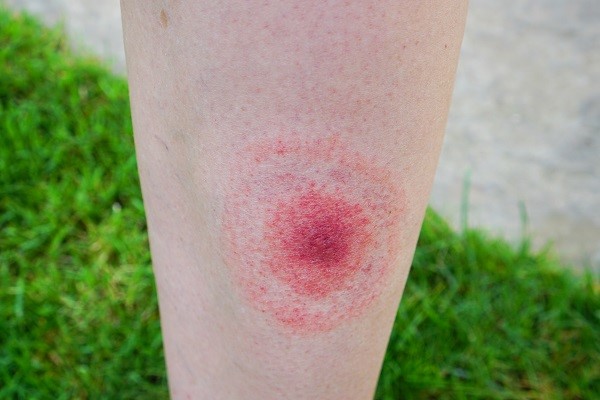
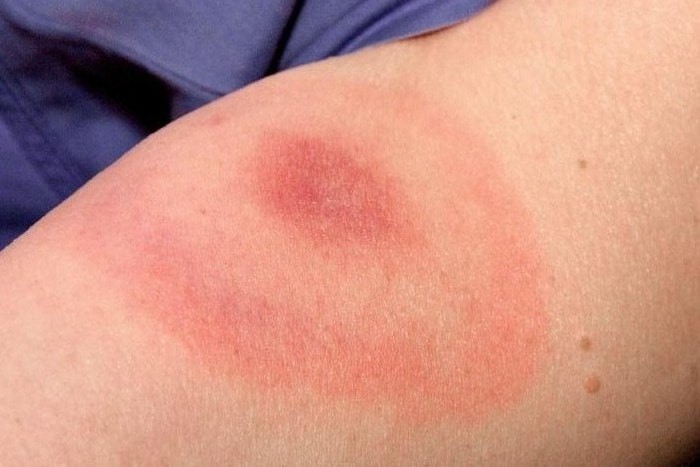
- erythema migrans, which occurs a few days to a few weeks after the parasite bite. In addition to the irritation that may be generated at the exact site of the bite, a characteristic ring shape is created around the bite, with darker and redder edges, while the inner area surrounding the bite remains lighter. It is called erythema migrans because it ‘migrates’ and spreads outwards. Usually there is only one erythema migrans, but in rare cases of multiple bites, true erythema can occur in the vicinity of all the tick sites. Given the very unusual form of this rash, the history should suggest at least the possibility of Lyme disease.
- Borrelia lymphocytoma: this is an asymptomatic, reddish-coloured, papular-nodular lesion in relief that occurs predominantly
- in children: on the face and in particular at the level of the ear lobe;
- in adults: on the nipple areola and scrotum.
Stage 2: Systemic spread
At a later stage the infection, if left untreated, can spread throughout the body with symptoms such as:
- fever;
- chills;
- muscle pain (myalgia);
- joint pain (arthralgia);
- headaches;
- severe tiredness and weakness (asthenia)
- burning and itching caused by light and heat (photophobia)
Stage 3: severe effects
In an even more advanced stage, then, the neglected and persistent infection can generate serious complications such as:
- arthritis
- encephalomyelitis, an inflammatory disease of the central nervous system, i.e. the brain and spinal cord;
- chronic atrophying acrodermatitis: a dermatitis that occurs mainly on the legs and lower limbs and initially presents with a violet, ill-defined erythema associated with oedema, while in the final stages it also presents with atrophy of the epidermis and dermis. The onset of chronic atrophying acrodermatitis occurs months to years after infection;
- peripheral neuropathy, i.e. damage to and malfunction of the peripheral neurological structures that connect the various parts of the body to the central nervous system, the symptoms of which often accompany chronic atrophying acrodermatitis;
- cardiac inflammation (carditis);
- meningitis.
Lyme disease: what to do if you are bitten by a tick
If you are immediately aware that you have been bitten by a tick, you should remove the parasite immediately, before it can transmit the spricocheta borrelia or other pathogens, using tweezers and taking care to avoid breaking the inoculated part, which may remain in the skin and cause infection.
If you are unable to do this, contact your doctor.
A patient who is bitten and has no symptoms is kept under observation and after a few weeks a blood test may be considered to see if an antibody to the spricocheta borrelia has developed.
Diagnosis and treatment of Lyme disease
Diagnosis is essentially clinical and when the patient presents with skin lesions compatible with Lyme disease, a biopsy can be performed and from this a cultural examination or other more advanced molecular biology tests can be carried out which can highlight the presence of the bacteria.
Once the diagnosis has been made, this is done:
- if the infection is still localised to the skin and joints, the treatment is in most cases oral antibiotic therapy based on doxycycline as the first line. In the case of pregnant women, allergies or minor patients, other choices may be amoxicillin, for example;
- for more advanced stages with multisystem involvement (in particular of the central nervous system), treatment is generally always antibiotic; usually based on ceftriaxone and administered intravenously;
- for more severe phases of protracted and undiagnosed infection, the treatment approach varies depending on the organ(s) involved and how much is involved.
How tick contact occurs
As the ISS(1) reminds us, the tick is a parasite that cannot jump or fly, but sits on top of vegetation, waiting for the animal or human organism to pass by and cling to, which it detects thanks to its ability to sense heat and carbon dioxide.
The areas of the body it bites and into which it creeps are generally:
- lower limbs;
- groin;
- armpits.
It remains in the area to which it attaches for a period of several days, during which it feeds on blood.
The bite is usually painless, as the tick’s saliva contains anaesthetic and anti-inflammatory principles that facilitate feeding.
This explains why it is very often not easy to detect the disease once the parasite vector has detached.
Where are ticks found?
Contact with ticks occurs mainly through
- woodland environments: places with a lot of grass and vegetation such as deciduous woods, grasslands, heaths and urban parks.
- stables and animal shelters: ticks are not very selective as to the hosts on which they feed, so they attach themselves to hares, squirrels, deer, dogs, cats, etc. that frequent the vegetation in which they are present. For this reason, care should always be taken when having contact with or visiting places where there are animals that have been in the vegetation.
How to prevent tick bites and Lyme disease
To prevent tick bites and, consequently, Lyme disease, advice is as follows:
in the countryside or wooded places:
- spray specific repellent products on your exposed skin;
- wear opaque clothing to avoid contact with grasses and brushwood (long-sleeved clothing, long trousers, socks and ankle-length shoes);
- carry out a thorough body inspection at the end of an activity in nature.
at home and in places frequented by animals that come into contact with vegetation:
- check the fur of the animals in question frequently, especially after a walk in the park or in environments with vegetation, their kennels and places where they play.
- Where possible, apply protective pesticides to animals at regular intervals so that they are always protected.
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
What To Do In Case Of A Snakebite? Tips Of Prevention And Treatment
Insect Bites And Animal Bites: Treating And Recognising Signs And Symptoms In The Patient
How To Protect Yourself From The Bite Of The Violin Spider (Or Brown Recluse)?