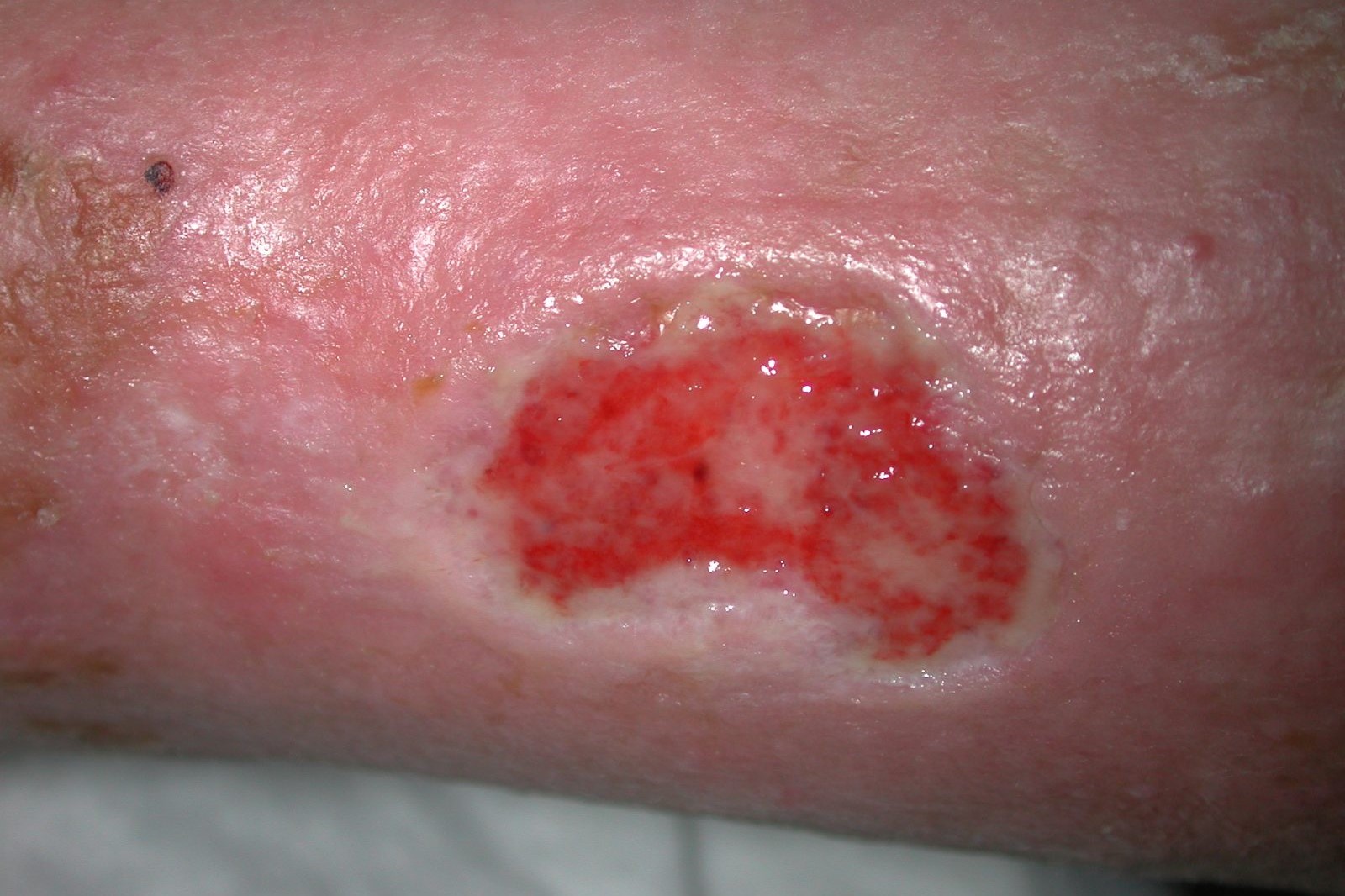
Why do skin ulcers occur?
How do these skin lesions occur and how can they be treated? Skin ulcers are lesions of the skin caused by delayed or failed healing
In 70% of cases these are ulcers of vascular origin, mainly venous, affecting mainly the legs and feet.
However, the causes of this disease are not always adequately investigated and it is often the case that ulcers are not properly considered and treated.
Skin ulcers, the symptoms
The symptoms that can occur are
- pain, caused by exposure of the deep epithelium and inflammatory processes;
- irritation;
- hyper-sensitivity;
- swelling;
- oedemas, from bleeding and redness, localised in the affected area.
The causes of skin ulcer formation
When the venous system malfunctions, skin ulcers can occur.
At one time, it was thought that this disorder could only belong to a certain category of people, the elderly.
However, with changing lifestyles, mainly focused on sedentary lifestyle and poor diet, skin ulcers can also occur in younger people.
The main causes are
- incorrect lifestyles (poor diet, smoking, sedentary lifestyle);
- pathologies such as diabetic foot, immune and systemic pathologies, neuropathies;
- decubitus injuries;
- surgery;
- traumas;
- burns.
It is important to know the cause of these open wounds, otherwise the correct course of treatment cannot be undertaken.
Types of skin ulcers
Generally, ulcers can be divided into acute and chronic.
Acute ulcers
Acute ulcers can result from:
- road traffic accidents
- burns;
- surgery.
Chronic ulcers
Chronic ulcers can be:
- related to: diabetic foot, decubitus, skin tumours, autoimmune and systemic diseases (connective tissue diseases).
- Vascular: these are the most frequent (70% of cases), the cause being poor venous circulation of the blood which leads to a reduced or absent supply of blood, and therefore oxygen, to the tissues.
- Vascular ulcers can be divided into venous and arterial ulcers.
Venous ulcers and arterial ulcers
Venous ulcers are linked to a malfunction of the venous system, chronic venous insufficiency, which leads to a certain stagnation of blood in the lower parts of the leg, with the appearance of swelling, superficial capillaries, varicose veins and, in the most serious cases, ulcers.
This type of lesion is characterised by
- the appearance of ‘map-like’ margins;
- the tendency to feel less pain and swelling when the legs are lifted.
Then there are arterial ulcers related to peripheral arterial disease.
This condition is characterised by narrowing or occlusion of the arteries resulting in poor oxygenation of the tissues, which suffer, leading to cell death and the appearance of lesions on the skin.
This type of lesion
- has very sharp edges;
- tends to improve by holding the legs downwards.
In both cases, if a secretion is present, especially one that smells unpleasant or is very profuse, it may be indicative of an infection or a lymphatic ulcer: any skin lesion that is struggling to heal should be an alarm bell for a specialist.
Diagnosis
Diagnostic tools used by the vulnologist include:
- acoustic mini doppler, a tool that can intercept a suspected arterial problem and thus refer the patient to the vascular surgeon;
- monofilament test, which is used to diagnose foot sensitivity in diabetic patients and detect possible nerve damage to refer the patient to a neurologist for further investigations;
Ankle-arm index or ankle-brachial index (ABI), also known as Winsor’s index, which is the ratio of systolic pressure measured at the ankle to that obtained at arm level. It measures the global vascularisation of a limb and is used as the first non-invasive screening test for the diagnosis of peripheral obliterative arterial disease (AOP).
Treatment and therapy
In order to treat these lesions properly it is best to go to a specialised vulnology centre: the specialist, called a vulnologist, will first of all take a careful history of the patient to check the possible causes of the ulcer.
Often, in fact, the ulcer can be the symptom of more complex pathologies (such as, for example, autoimmune or systemic diseases) or pathologies not yet diagnosed by the patient (such as, for example, type 2 diabetes).
Understanding the origin of the ulcer will allow the specialist to find, together with the patient, the most suitable pathway for managing the wound until it heals.
Today, there are different approaches to treating ulcers.
![]() Dressings
Dressings
Dressings, which are divided between traditional and technologically advanced dressings, vary depending on the objective:
- to clean the wound
- to reactivate the healing process
- eliminate bacteria;
- to keep the base of the wound moist.
Skin ulcers, the remedies
As possible solutions, there are also a number of adjuncts which serve mainly to reactivate the healing process and support the formation of new tissue.
These include
- local oxygen therapy with specific creams;
- devices that release oxygen locally and continuously (polarised light);
- gels that release ozone, which in turn is gradually transformed into oxygen;
- negative topical pressure devices that reactivate the healing process by forming new tissue.
Regenerative medicine
There is also regenerative medicine which is based on the use of products or techniques that can help regenerate ulcerated tissue, such as:
- PRP or MNC – Platelet-rich plasma or monocytes;
- purified, dried and treated northern cod skin containing re-epithelialisation stimulants;
- glass powder (bioglass) in combination with a vial of autologous blood;
- collagen (in solid or liquid form);
- natural carob derivatives.
Medicines
Finally, as a possible solution there are drugs, either to control the pain or to be used in case of ulcer infection.
It should be noted that local antibiotics are contraindicated, while systemic antibiotics are reserved for very selected cases.
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Wound Care Guideline (Part 1) – Dressing Overview
Wound Care Guideline (Part 2) – Dressing Abrasions And Lacerations
Wound Care Guideline (Part 3) – Pressure Wound Dressing
Wound Care Guideline (Part 4) – Leg Ulceration Dressing
Wound Care Guideline (Part 5) – Will The Wound Completely Heal