Anaphylactic shock: what it is and how to deal with it
Wasp and bee stings, drugs, foods such as peanuts: these are some of the most common causes of anaphylactic shock (or anaphylaxis), the most severe of all allergic reactions which, if not dealt with promptly, can even be fatal
Although, fortunately, the mortality rate remains low, the frequency of hospitalisations for anaphylaxis, in particular induced by food and drugs, has been increasing in recent years.
From allergy to anaphylactic shock
Allergy is a very common condition: it is estimated that 15% of the general population will suffer some type of allergic reaction during their lifetime.
The immune system recognises a normally harmless foreign substance (allergen) as an aggressive agent to be defended against, triggering a violent hypersensitivity reaction.
Allergy symptoms
Allergic symptoms vary depending on the mode of exposure, but generally allergy manifests itself with rhinitis or rhinoconjunctivitis, asthma, contact dermatitis, urticaria and/or angioedema, gastrointestinal disturbances, such as nausea, vomiting, diarrhoea and general malaise, hypotension, loss of consciousness and in severe cases, anaphylactic shock.
What is anaphylactic shock
Anaphylactic shock, or anaphylaxis, is the most severe and dangerous form of allergy.
At the basis of this reaction, as for all allergies, is the interaction between IgE and allergen, i.e. a substance that in predisposed persons can provoke the production of antibodies, called IgE.
These antibodies, after initial contact, attach themselves to the surface of certain cells, mast cells and basophils, which contain large amounts of histamine and other substances that can cause inflammation.
When the allergen comes into contact with the predisposed person’s body for the second time, it will encounter IgE fixed on the surface of the basophils and mast cells, causing the release of large amounts of histamine and inflammatory mediators responsible for anaphylactic shock.
The characteristics of anaphylactic shock, compared to ‘normal’ allergy, are:
- acute onset of the reaction: from a few minutes to a few hours after contact with the substance to which one is allergic;
- involvement of more than one system, i.e. skin, mucous membranes or both (e.g. with generalised urticaria, itching or flushing, swelling of the lips-tongue-upper throat), which may be associated with respiratory impairment (dyspnoea, wheezing-bronchospasm, stridor, hypoxia) or reduced blood pressure and associated symptoms of organ dysfunction (hypotension, loss of consciousness, syncope).
Symptoms of anaphylactic shock
The most frequent symptoms, present in more than 90% of cases, are skin and mucous membrane symptoms, followed by symptoms involving the respiratory and cardiovascular systems (in more than 50% of cases).
Less commonly, gastrointestinal symptoms may appear, such as nausea, vomiting, diarrhoea, abdominal cramps.
Usually, these symptoms are anticipated by tingling and a sense of warmth in the head, hands and feet.
Causes
Among the substances that can most commonly cause anaphylactic shock are:
- bee and wasp venom;
- foods, such as dried fruits (peanut, walnut, hazelnut, etc.), soy, shellfish and fish, milk and eggs;
- latex and related fruits: banana, avocado, kiwi, chestnut;
- drugs, such as antibiotics (especially penicillins and cephalosporins), non-steroidal anti-inflammatory drugs (NSAIDs)
- substances used for general anaesthesia and contrast media, such as those used in diagnostic imaging examinations;
- monoclonal antibodies.
In some cases, the triggering of the reaction is triggered by the presence of a cofactor, such as exercise, stress, infection, non-steroidal anti-inflammatory drugs and alcohol.
What to do in case of anaphylactic shock
In case of signs of anaphylactic shock, the first thing to do is to seek medical attention immediately and without wasting time, by calling Emergency Number or going to the emergency room.
If this is not possible or while waiting for help, it is advisable to
- remove or remove the trigger;
- place the person lying down with their legs elevated to ensure adequate venous return. In the case of pregnancy, the person can be placed on their side; in the case of respiratory distress while lying down, the person can be seated with their legs raised;
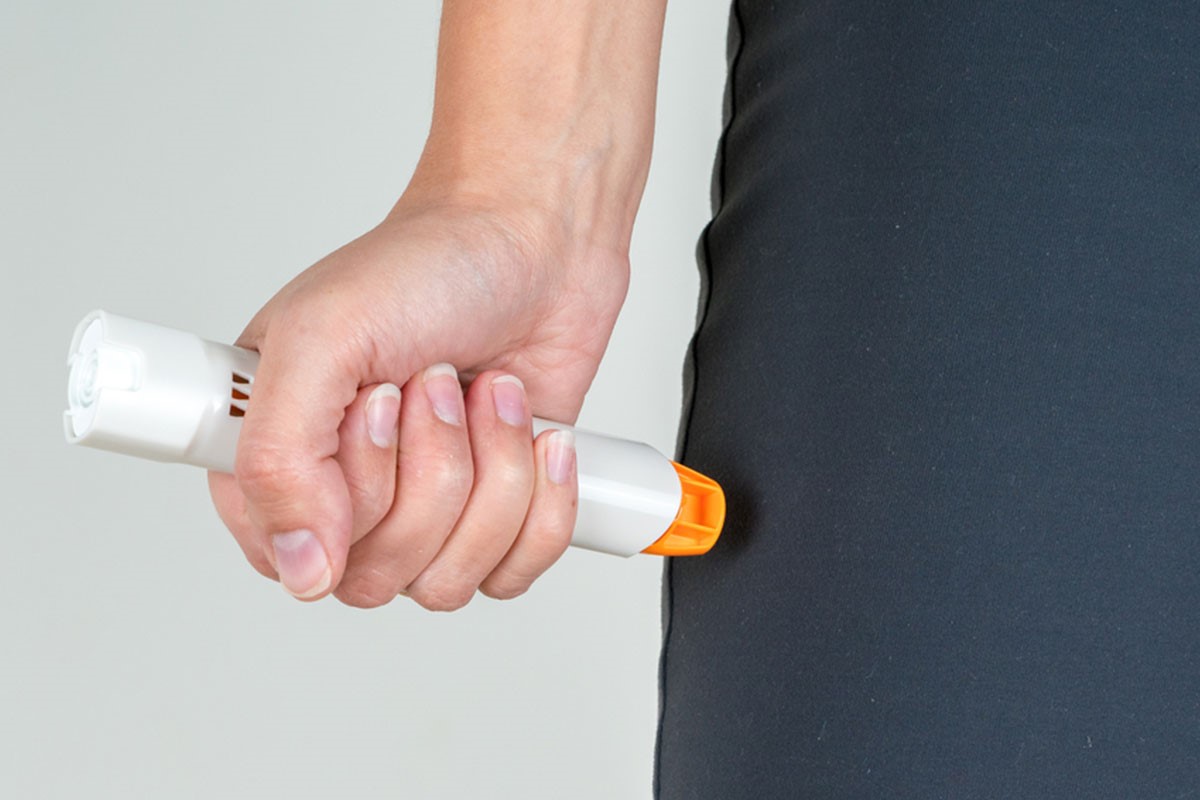
- if available, administering adrenaline (epinephrine) early via an auto-injector: this device, often prescribed for people with potentially severe allergies or who have already experienced anaphylaxis, consists of a syringe with a small, concealed needle that, when pressed against the thigh, injects a dose of the drug. The immediate use of an auto-injector can be a lifesaver in many cases.
Other drugs used, again with a doctor’s prescription, to counteract anaphylactic shock are:
- intravenous antihistamines and cortisone, to reduce airway inflammation and improve breathing;
- beta-agonists, e.g. albuterol, to relieve respiratory symptoms.
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Anaesthesia And Allergic Reactions: Factors To Take Into Account
Does The Recovery Position In First Aid Actually Work?
Insect Bites And Animal Bites: Treating And Recognising Signs And Symptoms In The Patient
What To Do In Case Of A Snakebite? Tips Of Prevention And Treatment
Wasps, Bees, Horseflies And Jellyfish: What To Do If You Get Stung Or Bitten?
What Should Be In A Paediatric First Aid Kit
Wasp Sting And Anaphylactic Shock: What To Do Before The Ambulance Arrives?


