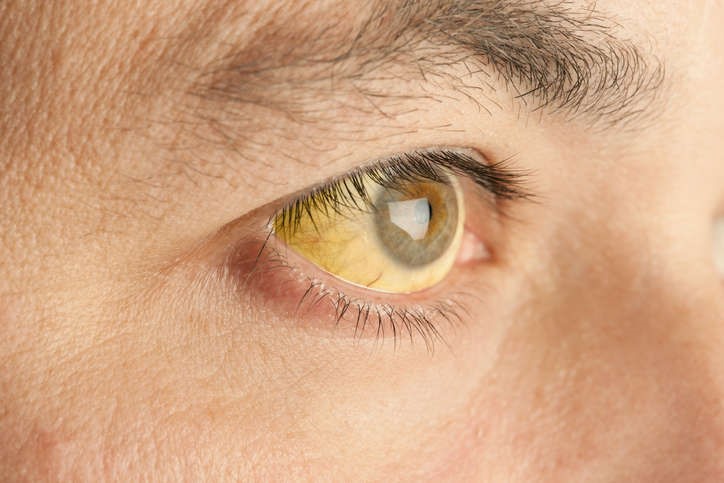
Haemolytic, cholestatic, obstructive, neonatal jaundice: an overview
Jaundice in medicine is a sign characterised by yellowish discolouration of the skin, sclerae and mucous membranes caused by excessively high levels of bilirubin, i.e. bilirubin in the blood
For jaundice to be visible, the bilirubin level must exceed 2.5 mg/dL.
Mild jaundice (sub-utterus), which can be observed by examining the sclerae under natural light, is usually detectable when serum bilirubin values are between 1.5 – 2.5 mg/dL.
Jaundice is a paraphysiological condition in newborns, whereas it is frequently a sign of pathology in adults.
Bilirubin derives from the catabolism of heme (a molecule contained in haemoglobin), and is present in the human body in two forms: an indirect form, which is normally found in the circulation and is carried by plasma albumin; and a direct form, in which bilirubin is conjugated with glucuronic acid, an indication that it has been glucoronically conjugated by the liver and rendered hydrophilic, suitable for elimination with bile.
Identifying which of the two forms of bilirubin is present in excess gives an indication of the cause of jaundice.
Jaundice should not be confused with a similar form of yellowish discolouration of the skin called ‘carotenoderma’ or ‘pseudo- jaundice’.
Haemolytic jaundice (with unconjugated or indirect hyperbilirubinaemia)
It is due to increased bilirubin production and/or an inability of the liver to carry out the conjugation process with glucuronic acid.
Bilirubin production increases in the course of haemolysis, i.e. increased destruction of red blood cells.
This occurs in certain blood diseases:
- increased oxidative stress in conjunction with red blood cell enzyme deficiencies (such as G6P-DH deficiency, glucose-6-phosphate dehydrogenase, commonly known as ‘favism’);
- transfusion of incompatible blood;
- autoimmune haemolytic anaemia;
- neonatal haemolysis by immunisation in the first pregnancy of Rh- mothers who conceive Rh+ children again;
- Gilbert syndrome or Crigler-Najjar syndrome.
Cholestatic jaundice (with conjugated or direct hyperbilirubinaemia)
This is due to cholestasis, a condition in which bilirubin is normally produced and goes to make up bile, but it encounters an obstacle and cannot travel the normal route that would take it into the intestines and thus be eliminated with the faeces.
This leads to other symptoms and signs that co-exist in these types of jaundice:
- marsala-coloured (or coke-coloured) urine; this is due to the fact that direct bilirubin, being water-soluble (unlike indirect bilirubin), once in the circulation can be eliminated with the urine, giving it its characteristic colour
- hypocolic or acholic faeces. Due to the fact that the colour of stools is normally given by bile pigments, which in this situation do not reach the intestine
- itching. In fact, bile salts are also present in the bile, which tend to be deposited in the skin when they circulate, giving intense itching.
By far the most frequent cause of cholestatic jaundice is gallstones, when a stone becomes wedged in the bile duct causing an obstruction in the outflow of bile, and thus jaundice.
Although hypocolic stools and bilirubinuria are characteristic of cholestatic jaundice, they can also occur in other non-obstructive intra-hepatic diseases and are therefore not sufficient signs for a diagnosis.
The main causes of obstructive jaundice are:
- neoplasms of the biliary tract and intestine;
- stones;
- papillitis;
- oddites;
- chronic pancreatitis;
- cysts;
- extrahepatic biliary tract neoplasms;
- compressions from external abnormal masses, such as carcinoma of the head of the pancreas;
- Dubin-Johnson syndrome;
- Rotor syndrome.
Neonatal jaundice
Neonatal jaundice is usually considered to be physiological and is caused by increased haemocateresis, i.e. destruction of haematous cells, such that it is not supported by the liver’s capacity as the liver is still immature.
It is observed in approximately 50% of term infants and in 80% of preterm infants.
It occurs on the second/third day and may last up to 8 days in term infants and up to 14 days in preterm infants.
Bilirubin levels usually settle without any intervention.
Infants with neonatal jaundice are treated with exposure to intense blue light (phototherapy).
Neonatal jaundice can cause permanent damage when its concentration exceeds 20-25 mg/dl, i.e. in the case of Kernicterus as bilirubin has toxic effects on the central nervous system.
Treatment of jaundice
While neonatal jaundice is considered a pseudo-physiological form that is reversible a few days after birth, and therefore not a particularly dangerous condition, jaundice manifested during adulthood is more alarming and is generally an indicator of an ongoing disease that may be more or less serious and treatable.
Infants who manifest jaundice are generally not subjected to any treatment; only in some cases are young patients exposed to phototherapy.
Only in rare circumstances is neonatal jaundice considered pathological; for example, when it appears as early as the first day of life, when the direct bilirubin concentration exceeds 1.5-2 mg/dl, or when the condition persists for more than two weeks.
In problematic cases, intravenous doses of albumin can be administered to prevent bilirubin deposition in the tissues, and sometimes phenobarbital.
Jaundice occurring during adulthood – as mentioned earlier – is more problematic.
In the case of jaundice, it is recommended to undergo all the necessary investigations to isolate the underlying cause: since the aetiology can be very varied, there is no single cure for all jaundice and only once the underlying cause has been identified can a specific therapy be administered.
The therapies can be very varied and include watchful waiting, a change in eating habits (in the case of gallstones or in the case of pseudo-uttering), one or more drugs and surgery (e.g. in the case of pancreatic cancer).
The following are the most commonly used drug classes in the treatment of jaundice
- Phenobarbital (e.g. Luminal, Gardenal, Phenoba FN): this drug belongs to the anticonvulsant class and is also used to treat pathological jaundice in infants and children under 12 years of age. As a guideline, a dose of 3-8 mg/kg per day is recommended, possibly divided into 2-3 doses. Do not exceed 12 mg/kg per day. Consult your doctor.
- Albumin (e.g. Album.Um.Immuno, Albutein, Albital): available as a solution to be injected intravenously, albumin is used in therapy for the treatment of jaundice, especially neonatal jaundice. The drug is indicated to hinder the accumulation of bilirubin in the tissues. Dosage and duration of treatment are the sole responsibility of physicians.
Medications used in therapy to treat gallstone-dependent jaundice
- Chenodeoxycholic acid: this is the most important bile acid produced by the liver. The active ingredient is used in therapy to help dissolve gallstones, also in the context of jaundice; treatment with this drug is able to partially or completely dissolve gallstones (consisting of cholesterol), thus resolving gallstone-dependent jaundice. Consult your doctor for dosage and method of administration.
- Ursodeoxycholic acid or ursodiol (e.g. Ursobil HT, Ursodes AGE, Litursol): administration of these drugs has been shown to be particularly suitable for dissolving gallbladder cholesterol stones, also in the context of jaundice. The recommended dosage is as follows: 8-12 mg/kg per os per day, as a single dose, in the evening or in two divided doses; extend therapy for up to two years (maintenance therapy: 250 mg per day). Adherence to the drug’s mode of intake is indispensable for curing the disease (calculi) and eliminating side effects (in this case, jaundice).
Medications used in therapy for mononucleosis-dependent jaundice
- Acyclovir (e.g. Acyclovir, Xerese, Zovirax): in certain cases of mononucleosis, possibly associated with jaundice, the doctor prescribes this substance, the drug of choice for the treatment of herpes simplex.
- Ibuprofen (e.g. Brufen, Moment, Subitene) the drug is an anti-inflammatory/analgesic (NSAID): it is recommended to take 200 to 400 mg of the active ingredient per os (tablets, effervescent sachets) every 4 to 6 hours, as needed. In some cases, the analgesic can also be administered intravenously (400 to 800 mg every 6 hours, as needed).
Read Also
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Bilirubin Encephalopathy (Kernicterus): Neonatal Jaundice With Bilirubin Infiltration Of The Brain
Palpation In The Objective Examination: What Is It And What Is It For?
Acute Abdomen: Causes And Cures
Abdominal Health Emergencies, Warning Signs And Symptoms
Abdominal Ultrasound: How To Prepare For The Exam?
Abdominal Pain Emergencies: How US Rescuers Intervene
Positive Or Negative Psoas Maneuver And Sign: What It Is And What It Indicates
Abdominoplasty (Tummy Tuck): What It Is And When It Is Performed
Assessment Of Abdominal Trauma: Inspection, Auscultation And Palpation Of The Patient
Acute Abdomen: Meaning, History, Diagnosis And Treatment
Abdominal Trauma: A General Overview Of Management And Trauma Areas
Abdominal Distension (Distended Abdomen): What It Is And What It Is Caused By
Abdominal Aortic Aneurysm: Symptoms, Evaluation And Treatment
Hypothermia Emergencies: How To Intervene On The Patient
Emergencies, How To Prepare Your First Aid Kit
Seizures In The Neonate: An Emergency That Needs To Be Addressed
Abdominal Pain Emergencies: How US Rescuers Intervene
First Aid, When Is It An Emergency? Some Information For Citizens
Acute Abdomen: Causes, Symptoms, Diagnosis, Exploratory Laparotomy, Therapies


