Methicillin-resistant staphylococcus infections: symptoms, diagnosis and treatment
Methicillin-resistant staphylococcus infections can mainly be contracted in hospitals or other healthcare facilities, typically during invasive procedures (e.g. surgery or insertion of catheters into a vein)
It is less common to come into contact with this microbe outside hospital facilities: skin-to-skin contact with a person carrying the bacterium is sufficient. In this case, activities such as contact sports like wrestling, working in close contact with children or living in crowded environments can increase the risk of infection.
Symptoms and diseases associated with methicillin-resistant staphylococcal infections
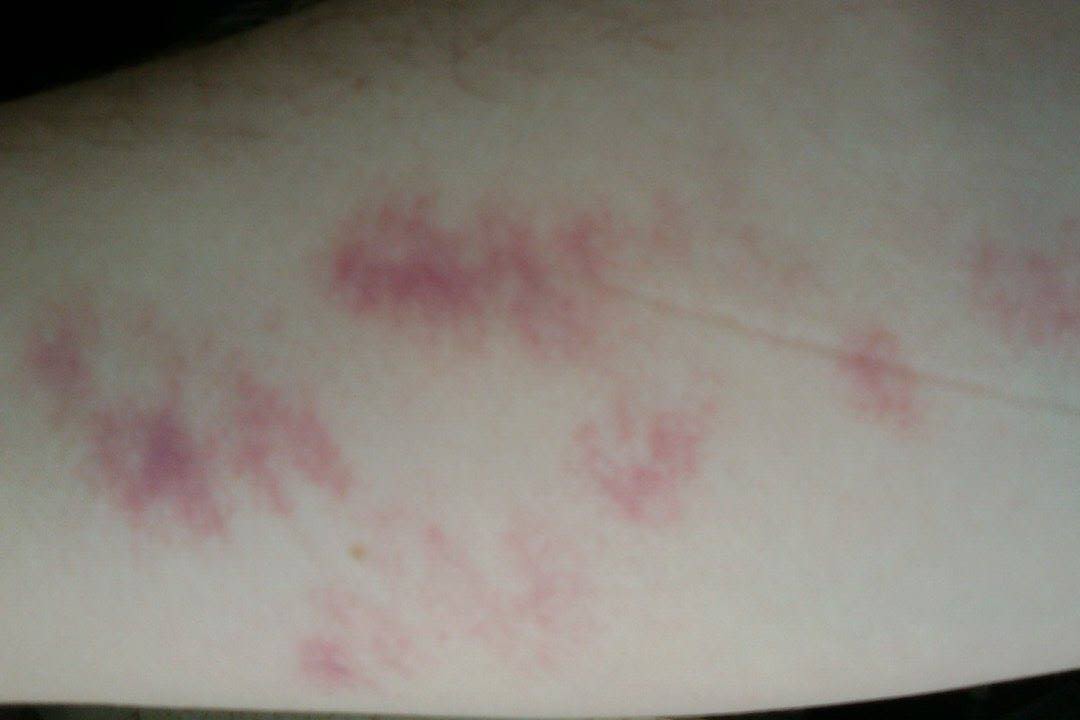
Typically, when they affect the skin, methicillin-resistant staphylococcal infections present as swollen, red, painful lumps that can look like boils or spider bites.
Possible symptoms associated with these swellings include:
- a warm sensation to the touch
- presence of pus or other filling material
- fever
- abscesses
However, methicillin-resistant staphylococcal infections can also strike deeper into the body, causing infections of:
- bones
- joints
- surgical wounds
- blood
- heart valves
- lungs
What are Methicillin-Resistant Staphylococcal Infections?
Methicillin-resistant staphylococcus is a type of Staphylococcus aureus that has developed resistance to many of the antibiotics normally used to treat Staphylococcus aureus infections.
Its emergence is believed to be the consequence of decades of inappropriate use of antibiotics, often prescribed unnecessarily to treat cold syndromes associated only with viruses (against which antibiotics are ineffective) and other diseases (such as influenza) that do not respond to treatment with these drugs.
More generally, heavy use of antibiotics increases the risk of resistance.
Care and treatment
Methicillin-resistant staphylococcal infections can be treated with antibiotics other than methicillin that manage to kill the microbe despite its resistance mechanisms.
However, not all infections require antibiotics. In some cases the doctor may, for example, opt for drainage of the abscess caused by the microbe without prescribing drugs.
Disclaimer: The information given here is general advice and in no way replaces medical advice. If you feel unwell, you should contact your doctor or go to the emergency room.
Read Also:
Antimicrobial Resistance In Europe – Data Seems More Dangerous Than Before
Pan-Resistance, Candida Auris In US Hospitals: Warning From CDC Atlanta
Vancomycin-Sensitive Staphylococcus Infections: Symptoms And Treatment


