Raynaud's phenomenon: causes, symptoms and treatment
Raynaud’s phenomenon is characterised by an excessive spasm of blood vessels in the periphery that causes a reduction in blood flow to the affected regions
The reaction can be triggered by cold and/or emotional stress (intense emotions, fright) and/or rapid change from warm to cold environments or other factors, some of which are still not fully understood.
Reduced blood flow results in numbness in the hands followed by cyanosis, pallor, pain, tingling and burning.
In half of the cases, the phenomenon may be secondary to other pathologies; if it is idiopathic (i.e. the reason for it is not known), it is called Raynaud’s syndrome, and is sometimes referred to as hypersensitivity or ‘allergy’ to cold.
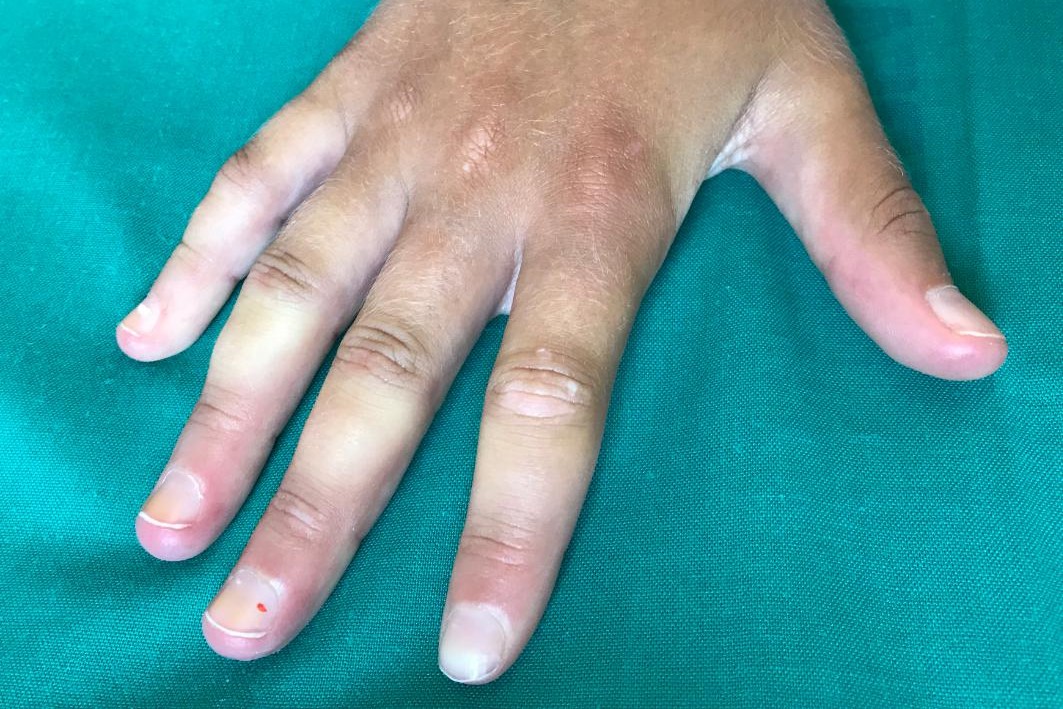
Raynaud’s phenomenon occurs mainly in the fingers and toes, but can also involve other areas of the body, such as the tip of the nose, earlobes and tongue
Raynaud’s phenomenon is named after the French physician Maurice Raynaud (1834-1881).
Causes and risk factors of Raynaud’s phenomenon
Pain is sometimes associated with it.
It is referred to as
- primary or primitive: the phenomenon occurs on its own, without an underlying disease causing it;
- secondary: the phenomenon is the sign of a pathology;
- idiopathic: if the underlying cause is unknown.
Primary Raynaud’s phenomenon is more frequent than the secondary form
Primary Raynaud’s usually begins under 25 years of age and mainly affects women who have an intolerance to cold that dates back to childhood.
On the other hand, patients with secondary Raynaud’s often present symptoms of an associated condition (typically arthritis, lupus, scleroderma…), such as joint pain, skin rashes and weakness.
Primary or idiopathic Raynaud’s phenomenon
Raynaud’s phenomenon is considered primitive or idiopathic if it occurs alone and is not associated with other diseases.
In this form it tends to occur frequently in young women and particularly during adolescence and early adulthood.
Idiopathic Raynaud’s is thought to be at least partly hereditary, although specific genes have not yet been identified.
Cigarette smoking is a factor that can increase the frequency and intensity of attacks; according to some authors, a hormonal component also seems to play a role.
Caffeine, oestrogen and non-selective beta-blockers are often listed as aggravating factors, but the evidence that they should be avoided does not appear solid.
Cold weather, mental and physical stress and intense emotions increase the risk of the phenomenon occurring.
Secondary Raynaud’s phenomenon
Raynaud’s phenomenon, or secondary Raynaud’s, is associated with a wide variety of other conditions and diseases:
- Connective tissue diseases
- Scleroderma
- Systemic lupus erythematosus
- Rheumatoid arthritis
- Sjögren’s syndrome
- Dermatomyositis
- Polymyositis
- Chronic agglutinin syndrome
- Ehlers-Danlos syndrome
- Drugs
- Beta-blockers
- Cytotoxic drugs – especially chemotherapeutics and especially bleomycin
- Cyclosporine
- Bromocriptine
- Ergotamine
- Sulfasalazine
- Drugs stimulating the central nervous system, e.g. amphetamines and methylphenidate
- Over-the-counter drugs, e.g. pseudoephedrine
- Occupational
- Prolonged hand exposure to chemical or plastic compounds, e.g. vinyl chloride, mercury or PVC
- Paraneoplastic manifestation
Other causes and risk factors:
- arteriopathy;
- nerve disorders;
- stroke-affected limb;
- multiple sclerosis;
- poliomyelitis;
- professional use of vibrating tools, such as pneumatic hammers, brush cutters or chain saws;
- carpal tunnel syndrome;
- upper thoracic strait syndrome;
- thyroid pathology;
- smoking;
- cold;
- injuries to hands or feet (fractures, surgery or frostbite).
Symptoms and signs
Raynaud’s phenomenon occurs mainly in those areas with greater caloric dispersion and lower metabolic demand (more expendable), i.e. the fingers (especially those of the hands).
In some cases, discomfort or pain is associated with the affected part.
It is characterised by three phases that can last from less than a minute to several hours in all
- Ischaemic (or ‘pallor’) phase: the blood supply is reduced and the area becomes pale, cold, numb and sometimes painful;
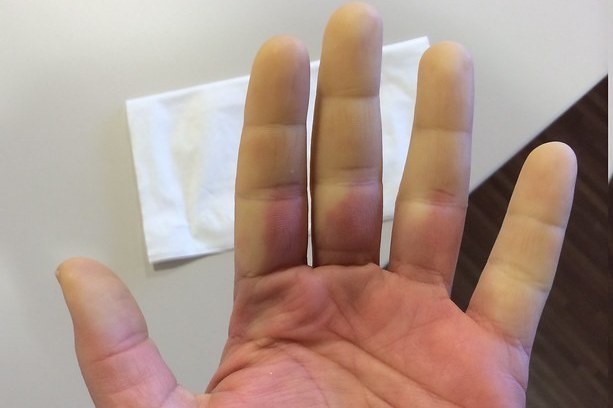
- Venous stasis phase (or ‘cyanosis’): the affected area begins to turn bluish and tingling and discomfort may be experienced;
- Reactive hyperemia phase (or ‘flushing’): blood flows back into the area profusely and the area appears reddish and is warm. Tingling, numbness and pain may occur. Normal flow usually resumes within a quarter of an hour.
In most cases, the phenomenon may interfere with the patients’ daily activities (especially those requiring the use of the hands or feet), but does not cause any long-term damage to the extremities.
Diagnosis
Diagnosis is essentially clinical: an objective examination allows the phenomenon to be detected, often without the need for cold stimulation tests.
Videapillaroscopy is the examination of first choice to distinguish idiopathic Raynaud’s phenomenon from that secondary to scleroderma spectrum diseases (scleroderma, polydermatomyositis, mixed connectivitis).
Video capillaroscopy in these patients shows typical changes: capillary loops reduced in number, avascular areas, giant capillary loops known as megacapillaries, microhaemorrhages.
The cold stimulation test involves immersing the patient’s hand in ice water to provoke an episode.
A compressive manoeuvre performed by the patient by pushing the palms against each other with the hands joined at prayer (signs that can be evoked in a more nuanced manner than with the cold stimulation test) can also be practised.
Complications of Raynaud’s phenomenon
Complications are rare.
They may occur:
- skin ulcers;
- scarring;
- gangrene;
- thin, tapered fingers with smooth, shiny skin;
- brittle and slowly growing nails.
Therapy
In patients suffering from Raynaud’s phenomenon, it is important to avoid exposure to the cold, using gloves and heavy socks to keep the extremities warm.
From a pharmacological point of view, in persons refractory to conservative treatment, calcium antagonists are very effective. They reduce the number and duration of episodes of vasospasm by inducing vasodilation of the peripheral arterioles.
In more severe cases, sympathectomy (endoscopic thoracic sympathectomy), a controversial surgical procedure, can be used.
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Psoriasis, An Ageless Skin Disease
Exposure To Cold And Symptoms Of Raynaud’s Syndrome
Psoriatic Arthritis: What Is It?
Psoriasis: It Gets Worse In Winter, But It’s Not Just The Cold That’s To Blame