Effective Airway Management and Ventilation: 10 Tips
Maintaining a patent BLS airway and securing an ALS airway via endotracheal intubation can be a dynamic and challenging endeavour, requiring coordinated efforts from multiple rescuers.
As such, it’s advantageous to use methods and techniques that help you achieve your goal of effective airway maintenance and ventilation.
Here10 tips in a stepwise progression that spans the spectrum through BLS to ALS airway management and ventilation.
- Place the patient in an optimal position to open the airway
The more open an airway is, the lower the ventilation pressure and volume required for effective ventilation. Richard Levitan, one of the first emergency medicine physicians to use an airway camera and the author of more than 20 airway management research articles, asserts that the creation of a patent open airway is a three-step process:
- Place the patient in a proper position;
- Insert an oral or nasal airway;
- Lift the mandible and submandibular structures.
- Use a BLS airway adjunct.
BLS airway adjuncts should be utilized in every patient receiving positive-pressure ventilation unless absolute contraindications for their use are present. It is a rare patient on whom you cannot use an oropharyngeal or nasopharyngeal airway.
- Use a jaw-thrust manoeuvre when opening the airway.
The jaw-thrust manoeuvre is an extremely effective way of lifting the jaw and hyoid, displacing them anteriorly, and lifting the tongue from the oropharynx, thereby preventing airway occlusion.
The jaw-thrust is highly effective when used with a BLS airway adjunct. In addition, it can be used in patients with suspected cervical spine injury whose cervical spines must be maintained in a neutral inline position.
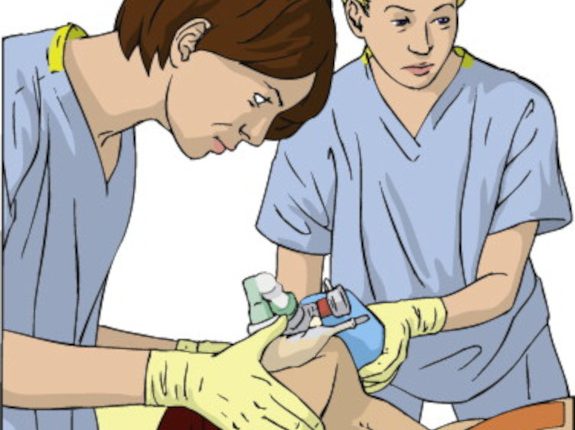
- Use two-rescuer BVM and the thenar eminence technique to obtain a good mask seal.
Obtaining an adequate mask seal on the patient’s face can be one of the more challenging components of airway maintenance and ventilation.
Whenever possible, bag-mask ventilation should be performed by two rescuers, one to hold the mask seal with two hands and the other to squeeze the bag-mask device at the appropriate rate.
Whenever possible, the rescuer with the most experience at maintaining airway patency should be responsible for the mask seal, and the less-experienced rescuer responsible for ventilation.
- Ventilate the patient using long inspiration times, with the smallest tidal volume required and as slow a rate as necessary to achieve optimal oxygenation.
The goal during BVM ventilation is adequate oxygenation without gastric insufflation or the generation of unnecessarily high intrathoracic pressure.
This is achieved by engaging in practices that avoid high airway pressures during BVM ventilation, such as optimal airway opening, longer inspiratory times, smaller tidal volumes and ventilating at as low a rate as possible.
- Position the patient for direct laryngoscopy and endotracheal intubation.
You’ve been ventilating a patient with a BVM and decided that endotracheal intubation is necessary. Is there an optimal position for direct laryngoscopy, one that best lines up the airway anatomy and ensures the best likelihood of a good look at the glottic opening and a better likelihood of success on the first pass?
The answer is yes, the head-elevated position. Positioning the patient with their ear canal on the same horizontal plane as their sternal notch maximizes the dimensions of the upper airway and facilitates direct laryngoscopy by bringing the pharyngeal and laryngeal axes into alignment, increasing the exposure of the glottic opening.
- Consider the use of apneic oxygenation during endotracheal intubation.
You’ve positioned your patient in preparation for direct laryngoscopy and an attempt at endotracheal intubation. You know that during your intubation attempt you will not be ventilating your patient (they will be apneic), and as a result, their SpO2 could fall.
Apneic oxygenation has been proven to extend the duration of apnea without hypoxia during rapid sequence intubation and is achieved by placing a nasal cannula on a patient and delivering oxygen at 15 lpm during the intubation attempt.
- Use external laryngeal manipulation to achieve the best view of the larynx possible.
It has clearly been shown that external laryngeal manipulation (ELM) can improve the view of the larynx during endotracheal intubation. Two ELM methods are commonly employed: bimanual laryngoscopy and the BURP manoeuvre.
Bimanual laryngoscopy (so named because the laryngoscopist uses two hands in the procedure) involves external manipulation of the patient’s larynx with the laryngoscopist’s right hand while the left holds the laryngoscope.
The BURP (backward, upward, rightward pressure) manoeuvre is performed independently by an assistant while the laryngoscopy is performed by his partner. It is, in a sense, performed blindly in anticipation that the displacement will result in a better view of the larynx.
- Use an endotracheal tube introducer.
An endotracheal tube introducer, commonly called a bougie, is a simple and inexpensive way to increase the success rate of your endotracheal intubation attempts. It is most effective in situations where only the epiglottis is visible, not the vocal cords or arytenoids.
How effective is the bougie at increasing endotracheal intubation success rates? In one study, the endotracheal intubation success rate improved from 66% with the use of stylet only to 96% with the use of a bougie.
- Confirm tube placement in the trachea using end-tidal carbon dioxide detection.
It has been shown that visualization of the endotracheal tube passing through the vocal cords is not a reliable method of confirming placement of an endotracheal tube into the trachea. In addition, auscultation of the chest for breath sounds, auscultation of the epigastrium for the absence of air ventilation sounds in the stomach, and the observation of chest wall movement during ventilation are “notoriously inaccurate methods of confirming endotracheal tube placement.”
The standard for endotracheal tube placement confirmation, and the method recommended by the AHA, is continuous waveform capnography.



