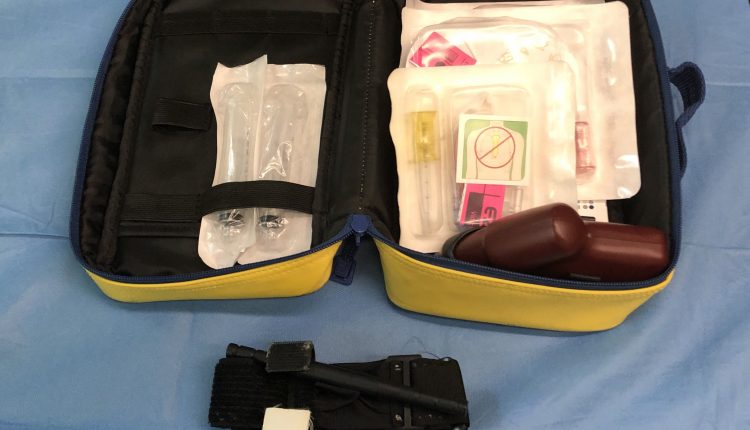
Tourniquet and intraosseous access: massive bleeding management
In case of massive bleeding, timely control of the bleed and immediate vascular access can make the difference between life and death of a patient. In this article, we will report an Italian case study on the use of a tourniquet and intraosseous access.
The emergency care system 118 of Trieste (Italy) has decided to assign the EZ-IO® intraosseous access device to all ALS ambulance services of the area. The aim is to equip ambulances in case of severe bleeding and to train medical practitioners working in the prehospital setting in the management of massive junctional and limb haemorrhages. They joined the “Stop the bleed” campaign, promoted by the American College of Surgeon and imported into Italy by the Società Italiana di Chirurgia d’Urgenza e del Trauma (Italian Society of Emergency Surgery and Trauma). The use of a tourniquet and intraosseous access can mean an important changing in treating such complicate bleeding.
Authors: Andrea Clemente, Mauro Milos, Alberto Peratoner SSD 118 Trieste – Department of Emergency (attività integrata di Emergenza, Urgenza ed Accettazione). Azienda Sanitaria Universitaria Giuliano Isontina
Intraosseous access: Tourniquet and massive bleeding
Every year, trauma is responsible for a significant percentage of mortality worldwide. The World Health Organization estimated that in 2012, 5.1 million people died because of traumatic events, which is like 9.2% of deaths worldwide (mortality rate verified in 83 cases per 100,000 inhabitants). 50% of the deaths were between the ages of 15 and 44, with a male mortality rate twice that of women(1).
In Italy, trauma events are responsible for 5% of total annual deaths (2). It corresponds to about 18,000 deaths, of which:
- road accidents: 7,000 deaths
- domestic accidents: 4,000 deaths
- accidents at work: 1,300 deaths
- acts of delinquency / or self-injury: 5,000 deaths
Many are caused by over 1 million hospital admissions, equal to about 10% of total annual admissions (3).
Haemorrhagic shock is the second leading cause of death after central nervous system injuries, regardless of the mechanism 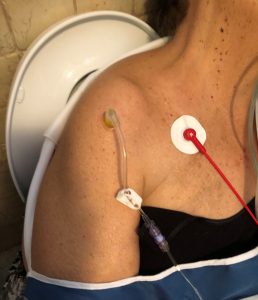 of trauma. Haemorrhage is responsible for 30-40% of trauma deaths and 33-56% occurs in an out-of-hospital setting (4).
of trauma. Haemorrhage is responsible for 30-40% of trauma deaths and 33-56% occurs in an out-of-hospital setting (4).
In order to be more effective as possible, the haemorrhage treatment has to be provided as soon as possible after the damage occurs. Massive bleeding can quickly lead to so-called “trauma triad of death” or “lethal triad”: hypothermia, coagulopathy and metabolic acidosis.
Massive bleeding decreases oxygen transport and can cause hypothermia with consequent alteration of the coagulation cascade. In the absence of oxygen and nutrients normally transported by the blood (hypoperfusion), cells switch to anaerobic metabolism, causing the release of lactic acid, ketone bodies and other acidic components that lower the blood pH causing metabolic acidosis. Increased acidity damages tissues and organs in the body and can reduce myocardial performance by further compromising oxygen transport.
Tourniquet and intraosseous access: life-saving manoeuvres
From the conflicts in Iraq and Afghanistan, we have learned that the immediate use of a tourniquet and hemostatic bandages are essential in life-saving manoeuvres. A very efficient way of responding, deeply studied by the US Army’s Committee on Tactical Combat Casualty Care (C-TCCC). The implementation of the TCCC guidelines has led to a significant reduction in the number of extremity haemorrhage deaths (5).
Thanks to a deep experience developed at a military level, these methods of treatment have begun to spread also in the civil setting, above all, following terrorist attacks such as that occurred during the Boston Marathon in 2013 (6).
Quick life-saving actions for the control of the haemorrhages by first responders, bystanders included, can mean a crucial point in the reduction of preventable deaths (7). In the United States, one of the strategies that have proven effective in reducing massive haemorrhage mortality has been to equip both health care personnel and first responders (police and firefighters) with haemorrhage control devices and training (8).
In common and daily emergency medical services, the compression bandage used in massive haemorrhage is often inadequate. It is effective only when direct manual compression is carried out, which cannot always be guaranteed in the event of multiple injuries or maxi emergencies (5).
That’s why many emergency organizations use a tourniquet. It has only one purpose: prevent hemorrhagic shock and massive bleeding out of a limb. It has been scientifically proven that its application is undoubtedly life-saving. Patients who experience traumatic hypovolemic shock have a statistically severe prognosis with low survival rates. Collected evidence in the military field has shown that injured people to whom tourniquet was applied before the onset of hypovolemic shock have a survival rate of 90%, compared to 20% when the tourniquet was applied after the first symptoms of shock (9).
Early use of tourniquet reduces the need for volemic reintegration with crystalloids in an extra-hospital environment (haemodilution, hypothermia) and hemoderivatives in a hospital environment (coagulopathies), avoiding further worsening the factors involved in the lethal triad (10).
During the Vietnam conflict, 9% of deaths were caused by bleeding. In today’s conflicts, it has been reduced to 2% thanks to training on the use of a tourniquet and its widespread diffusion. The survival rate among soldiers treated with tourniquet vs. those in which it was not applied is 87% vs. 0% (9). The analysis of 6 international studies reported an amputation rate of 19% of the limbs involved.
These amputations were probably caused by the large extent of primary injuries and not described as secondary complications to tourniquet use (11). In two major military studies, it was found that the rate of complications due to tourniquet use ranged from 0.2% (12) to 1.7% (9). Other studies showed an absence of tourniquet complications remaining in place between 3 and 4 hours (13.14).
We have to consider 6 hours as the maximum limit for limb survival (15). The “Stop the Bleed” campaign was promoted in the U.S. by a working group among various agencies convened by the Department of Homeland Security of the “National Security Councill Staff” of the White House, with the objective of building resilience among the population by increasing awareness of the basic actions to stop life-threatening bleeding caused both by accidental events of everyday life and by disastrous events of a natural or terrorist nature.
The “Committee on Trauma” of the American College of Surgeons and the Hartford Consensus are among the main promoters of this campaign. Uncontrolled bleeding is considered the leading cause of death preventable by trauma, while the cornerstone of timely intervention is the use of bystanders as first responders to manage massive bleeding until the arrival of professional rescue, after having ascertained that the intervention is effective within the first 5-10 minutes.
The practitioners of 118 Trieste system took part in the “Stop the Bleed” course, imported into Italy by the Società Italiana di Chirurgia d’Urgenza e del Trauma. The aim is to standardise behaviour on the correct use of the tourniquet, currently available on all the Province’s rescue vehicles.
About tourniquet and intraosseous access
In the pre-hospital setting, it is often essential to ensure rapid vascular access, but the positioning is often 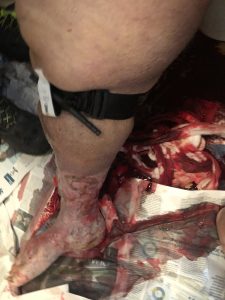 problematic (16,17). Peripheral venous access remains the standard, but if vital functions are compromised, its retrieval may be difficult or it may take too long.
problematic (16,17). Peripheral venous access remains the standard, but if vital functions are compromised, its retrieval may be difficult or it may take too long.
Environmental factors such as poor lighting, limited space, difficult patient or clinical factors such as peripheral vasoconstriction in shock or hypothermic patients, the poor venous assets due to intravenous therapy or obesity may make difficult to obtain peripheral venous access.
Victims of trauma with increased dynamics, cardiac arrest or sepsis may require immediate vascular access.
In pediatric patients, obtaining vascular access may be technically difficult (18). The success rate in positioning peripheral venous access at the first attempt outside the hospital is 74% (19.20) and is reduced to less than 50% in case of cardiac arrest (20). Patients in hemorrhagic shock require, on average, 20 minutes to obtain peripheral venous access (21).
Tourniquet and intraosseous access: the valid alternative to peripheral venous access is intraosseous access: it is obtained much faster than peripheral vein retrieval (50±9 s vs 70±30 s) (22). In the intra-hospital setting in ACR patients with unavailable peripheral veins, intraosseous access has shown a higher success rate in less time than CVC placement (85% vs 60%; 2 min vs 8 min) (23), moreover the procedure does not require the interruption of chest compressions and consequently could improve the patient’s survival (24).
The European Resuscitation Council also recommends intraosseous access as a valid alternative in case of failure to find the peripheral vein in the adult patient (25) and as the first choice in the pediatric patient (26).
As of April 2019, the EZ-IO® Intraosseous Access System was made operational on all ASUITS 118 Advanced Rescue Ambulances after training of nurses and dissemination of operating procedures, previously only the self-medication system was equipped.
The diffusion of the control to all ambulances makes it possible to quickly guarantee vascular access, reduce treatment times and further increase the quality of services for citizens. Several studies have shown that EZ-IO® is an effective intra-osseous access retrieval system: the overall success rate is very high (99.6%27; 98.8%28; 90%29) as well as the success rate at the first attempt (85.9%27; 94%28; 85%23) and is characterized by a very fast learning curve (29). Intraosseous access is equivalent to peripheral venous access in terms of pharmacokinetics and clinical efficacy (30) and the complication rate is less than 1% (24).
About the intraosseous access and the use of tourniquet, case report
Case report:
6.35 pm: the 118 Trieste system was activated by the FVG Regional Emergency Medical Operations Room to respond to a traumatic yellow code at home.
6.44 pm: the ambulance arrived on site and the crew was accompanied by the patient’s relatives in the bathroom. A 70-year-old obese woman, sitting on the toilet and unconscious (GCS 7 E 1 V2 M 4). Snoring breath, pale, diaphoretic, barely perceptible carotid pulse, capillary refill time > 4 seconds. A large blood slick at the feet of the patient; vascular ulcers were evident in the lower limbs and a towel, also soaked in blood, was wrapped around the right calf.
6.46 pm: red code. Self-medication was requested and they had to call for fire brigade assistance to assist the transport of the patient, considering her weight condition and the limited space available. When the towel was removed, a haemorrhage from a probable vascular rupture was detected in the ulcuscruris, located in the posterior part of the calf.
It was impossible to guarantee effective direct compression and to dedicate an operator for this purpose. So, they immediately applied the Combat Application Tourniquet (C.A.T.), stopping the bleeding. After that, no other hemorrhagic mouths were detected.
The head was hyper-extended and applied O2 with 100% FiO2 with the disappearance of snoring breath.
Given the state of shock and obesity, it was impossible to find peripheral venous access, so, after the first attempt, intraosseous access was placed in the right humeral chamber with EZ-IO® system with a 45mm needle.
The correct positioning of the access was confirmed: needle stability, serous blood aspiration and ease of infusing the 10 ml SF push. Physiological Solution 500 ml infusion with bag squeezer was started and the limb was immobilized with a mitella. When ECG monitoring was placed, 80 rhythmic HR, PA and SpO2 were not detectable.
A compressive medical dressing was then applied at the bleeding point. A rapid anamnestic collection showed that the patient was suffering from hyperthyroidism, arterial hypertension, dyslipidemia, OSAS in nocturnal CPAP, atrial fibrillation in TAO. She was also followed by Plastic Surgery and Infectious Diseases for lower limb ulcers with dermohypodermite by MRSA, P. Mirabilis and P. Aeruginosa and in therapy with tapazole 5mg 8 hours, bisoprolol 1.25mg h 8, diltiazem 60mg every 8 hours, coumadin according to INR.
6.55 pm; the automedicator arrived on site. The patient presented with GCS 9 (E 2, V 2, M 5), FC 80r, PA 75/40, SpO2 98% with FiO2 100%. 1000mg EV tranexamic acid was administered. With the help of the Fire Brigade, the patient was mobilized with a chair and then on a stretcher.
In the ambulance, the patient was presented with GCS 13 (E 3, V 4, M 6), PA 105/80, FC 80r and SpO2 98% with FiO2 100%. The right humeral intraosseous access was found to have dislodged during the mobilization phases, so another intraosseous access was immediately successfully placed in the left humeral seat and the infusion of fluids continued.
Given the improvement in vital parameters, analgesic therapy was performed with fentanest 0.1mg and a total of 500ml of saline and 200ml of ringeracetate were infused. At 7.25 p.m. the ambulance, with the doctor on board, left in code red to the Cattinara Emergency Room.
Surgeon, resuscitation department and blood bank were alerted. The ambulance arrived in PS at 7.30 p.m.
The first blood count showed: haemoglobin 5 g/dL, red blood cells 2.27 x 103µL, haematocrit 16.8%, while for coagulation: INR 3.55, 42.3 seconds, Ratio 3.74. The patient was admitted to emergency medicine and underwent hemotransfusions for a total of 7 units of concentrated hematocrits and antibiotic cycle with dalbavancin and cefepime.
Tourniquet, massive bleeding and intraosseous access: READ THE ITALIAN ARTICLE
READ ALSO
Tourniquet: Stop bleeding after a gunshot wound
Interview with AURIEX – Tactical medical evacuation, training and mass bleeding control
Tourniquet or no tourniquet? Two expert orthopaedics speak on the total knee replacement
Tactical Field Care: how should paramedics be protected to face a war field?
Tourniquet, massive bleeding and intraosseous access BIBLIOGRAPHY
1. World Health Organization. The magnitude and causes of injuries. 2–18 (2014). doi:ISBN 978 92 4 150801 8
2. Giustini, M. OSSERVATORIO NAZIONALE AMBIENTE E TRAUMI (ONAT) Traumi: non solo strada. in Salute e Sicurezza Stradale: l’Onda Lunga del Trauma 571–579 (C.A.F.I. Editore, 2007).
3. Balzanelli, M. G. Il supporto delle funzioni vitali al paziente politraumatizzato – Trauma Life Support (TLS). in Manuale di Medicina di Emergenza e Pronto Soccorso 263–323 (CIC Edizioni Internazionali, 2010).
4. Kauvar, D. S., Lefering, R. & Wade, C. E. Impact of hemorrhage on trauma outcome: an overview of epidemiology, clinical presentations, and therapeutic considerations. J. Trauma60, S3-11 (2006).
5. Eastridge, B. J. et al. Death on the battlefield (2001-2011): Implications for the future of combat casualty care. J. Trauma Acute Care Surg.73, 431–437 (2012).
6. Walls, R. M. & Zinner, M. J. The Boston Marathon response: why did it work so well? JAMA309, 2441–2 (2013).
7. Brinsfield, K. H. & Mitchell, E. The Department of Homeland Security’s role in enhancing and implementing the response to active shooter and intentional mass casualty events. Bull. Am. Coll. Surg.100, 24–6 (2015).
8. Holcomb, J. B., Butler, F. K. & Rhee, P. Hemorrhage control devices: Tourniquets and hemostatic dressings. Bull. Am. Coll. Surg.100, 66–70 (2015).
9. Kragh, J. F. et al. Survival with emergency tourniquet use to stop bleeding in major limb trauma. Ann. Surg.249, 1–7 (2009).
10. Mohan, D., Milbrandt, E. B. & Alarcon, L. H. Black Hawk Down: The evolution of resuscitation strategies in massive traumatic hemorrhage. Crit. Care12, 1–3 (2008).
11. Bulger, E. M. et al. An evidence-based prehospital guideline for external hemorrhage control: American College of Surgeons Committee on Trauma. Prehosp. Emerg. Care18, 163–73
12. Brodie, S. et al. Tourniquet use in combat trauma: U.K. military experience. J. Spec. Oper. Med.9, 74–7 (2009).
13. Welling, D. R., McKay, P. L., Rasmussen, T. E. & Rich, N. M. A brief history of the tourniquet. J. Vasc. Surg.55, 286–290 (2012).
14. Kragh, J. F. et al. Battle casualty survival with emergency tourniquet use to stop limb bleeding. J. Emerg. Med.41, 590–597 (2011).
15. Walters, T. J., Holcomb, J. B., Cancio, L. C., Beekley, A. C. & Baer, D. G. Emergency Tourniquets. J. Am. Coll. Surg.204, 185–186 (2007).
16. Zimmermann, A. & Hansmann, G. Intraosseous access. Neonatal Emergencies A Pract. Guid. Resusc. Transp. Crit. Care Newborn Infants39, 117–120 (2009).
17. Olaussen, A. & Williams, B. Intraosseous access in the prehospital setting: Literature review. Prehosp. Disaster Med.27, 468–472 (2012).
18. Lyon, R. M. & Donald, M. Intraosseous access in the prehospital setting—Ideal first-line option or best bailout? Resuscitation84, 405–406 (2013).
19. Lapostolle, F. et al. Prospective evaluation of peripheral venous access difficulty in emergency care. Intensive Care Med.33, 1452–1457 (2007).
20. Reades, R., Studnek, J. R., Vandeventer, S. & Garrett, J. Intraosseous versus intravenous vascular access during out-of-hospital cardiac arrest: A randomized controlled trial. Ann. Emerg. Med.58, 509–516 (2011).
21. Engels, P. T. et al. Use of intraosseous devices in trauma: A survey of trauma practitioners in Canada, Australia and New Zealand. Can. J. Surg.59, 374–382 (2016).
22. Lamhaut, L. et al. Comparison of intravenous and intraosseous access by pre-hospital medical emergency personnel with and without CBRN protective equipment. Resuscitation81, 65–68 (2010).
23. Leidel, B. A. et al. Comparison of intraosseous versus central venous vascular access in adults under resuscitation in the emergency department with inaccessible peripheral veins. Resuscitation83, 40–45 (2012).
24. Petitpas, F. et al. Use of intra-osseous access in adults: a systematic review. Crit. Care20, 102 (2016).
25. Soar, J. et al. European Resuscitation Council Guidelines for Resuscitation 2015: Section 3. Adult advanced life support. Resuscitation95, 100–47 (2015).
26. Maconochie, I. K. et al. European Resuscitation Council Guidelines for Resuscitation 2015. Section 6. Paediatric life support. Resuscitation95, 223–248 (2015).
27. Helm, M. et al. EZ-IO® intraosseous device implementation in German Helicopter Emergency Medical Service. Resuscitation88, 43–47 (2015).
28. Reinhardt, L. et al. Four years of EZ-IO® system in the preand in-hospital emergency setting. Cent. Eur. J. Med.8, 166–171 (2013).
29. Santos, D., Carron, P. N., Yersin, B. & Pasquier, M. EZ-IO® intraosseous device implementation in a pre-hospital emergency service: A prospective study and review of the literature. Resuscitation84, 440–445 (2013).
30. Von Hoff, D. D., Kuhn, J. G., Burris, H. A. & Miller, L. J. Does intraosseous equal intravenous? A pharmacokinetic study. Am. J. Emerg. Med.26, 31–38 (2008).


