Coccygodynia: symptoms, diagnosis and treatment
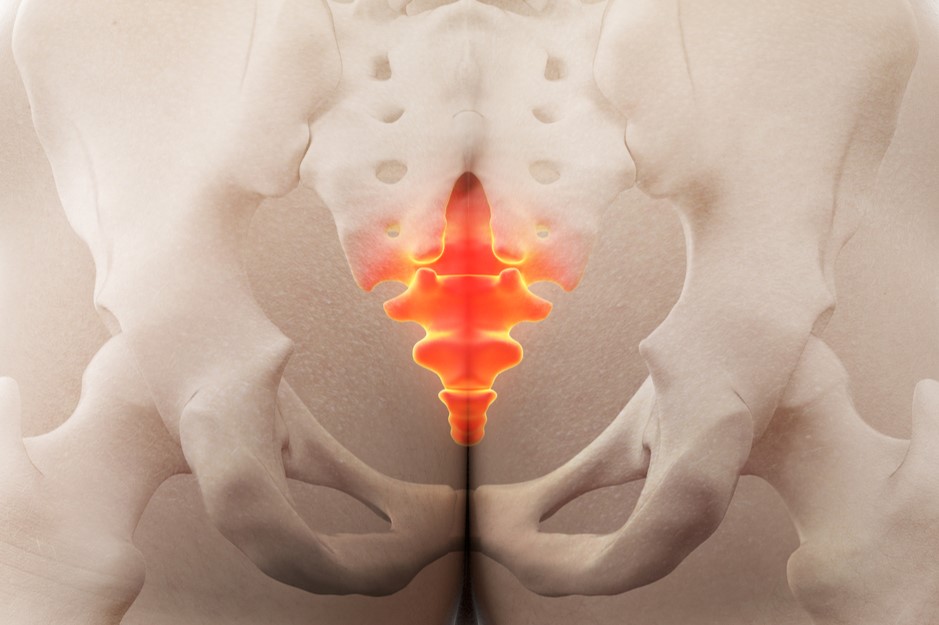
Coccygodynia is an intense pain in the coccyx and at the end of the lumbar spine. The pain that radiates in the lower back and sometimes makes it difficult even to sit down or perform mundane activities, such as tying one’s shoes, could be due to an inflammation of the coccyx: coccygodynia
What is coccygodynia?
Coccigodynia or coccidynia, from the Greek kòkkux = ‘coccyx’ and odùne = ‘pain’, does not refer to a specific pathology, but to a painful symptomatology originating from an inflammatory state at the end of the spinal column, the osteo-ligamentous region of the coccyx, located at the level of the anal region and gluteal fold.
Coccidynia mainly affects a population with an average age of 40 years, in 60-70% of cases female.
The reasons may lie in the greater prominence of the coccyx in women compared to men, thus in their greater susceptibility to this type of inflammatory state.
In addition, another element characterising the female prevalence of coccygodynia is its frequent association with the menstrual cycle and, in some cases, with trauma generated during childbirth.
Symptoms of coccygodynia
This syndrome manifests itself, as already mentioned, with pain in the coccyx region, which sometimes, however, also characterizes the neighbouring areas, such as the lumbar spine and buttocks, and may become more acute:
- in a sitting position;
- when moving from a sitting to a standing position;
- when pressure is applied to the affected area.
The causes
The underlying causes of this painful manifestation can be summarised as follows:
- direct trauma: a blow or an injury to the coccyx area can be the cause of inflammation, with the following statistical differentiations:
- trauma from a fall in about 25% of cases;
- mild but repeated trauma, such as in sports such as cycling and rowing, in about 12%;
- childbirth trauma, in about 12%;
- trauma from surgical treatment in about 5% (at least 50% of these from surgery performed in the ‘lithotomy position’, i.e. with the patient lying on his back with his knees apart).
- unknown cause (idiopathic);
- prostatitis: so as a result of an inflammation of the prostate.
- tumour: at the basis of coccygodynia there may, more rarely, also be a neoplasm such as, for example
- chordoma: a tumour which usually develops at the base of the neck or spine;
- giant cell tumour or osteoclastoma: bone neoplasm characterised by the presence of giant cells and occurring mainly in long bones such as the femur and tibia;
- intradural schwannoma: tumour affecting Schwanna cells in the spinal nerves;
- perineural cysts (Tarlov’s cysts): pockets containing cerebrospinal fluid that originate along the spinal column and in particular in the sacral area;
- intraosseous lipoma: fatty tissue that forms inside the bone;
- rectal carcinoma: cancer of the rectum, the part of the intestine closest to the anus;
- sacral hemangioma: a proliferation of the epithelial cells of the blood vessels in the sacral area;
- pelvic metastases, often from prostate cancer.
Diagnosis of coccygodynia
The diagnosis of coccygodynia is purely clinical, i.e. with the patient manifesting pain and/or soreness in the anal fold.
Confirmation is made by injection of local anaesthetic in the coccyx area: if the pain is related to that area, the subject will perceive immediate relief.
This is necessary for a differentiated history from pain in other areas within the lower spine and pelvic region that may simulate coccygodynia.
If the anaesthetic test is positive, dynamic radiography or MRI will follow, which will show if the coccyx is dislocated when the patient is about to sit.
Dynamic X-ray can identify the cause of pain in about 68% of patients, while bone scan and magnetic resonance imaging (MRI) can detect or exclude both bone fractures and neoplastic diseases.
If the diagnosis of coccydynia is suspected, referral should be made to a surgeon experienced in spinal surgery, i.e. a neurosurgeon or orthopaedist.
Remedies
The majority of patients show an improvement or even complete resolution of symptoms within 3 months of diagnosis of coccydynia, through conservative treatment, which is essentially based on
- drug therapy with: non-steroidal anti-inflammatory drugs; mild analgesics; muscle relaxants (myorelaxants);
- rubber cushion with the classic ‘doughnut’ shape, used to reduce pressure on the coccyx in the sitting position;
- lumbar bands and chairs with lumbar support, to maintain the required lordosis.
However, patients who experience improvement with conservative treatment in about 20% of cases may experience a recurrence of symptoms in the first year.
In these situations the choice may be to repeat conservative treatment or to implement more targeted strategies.
Coccygodynia therapy for refractory cases
For the most obstinate clinical cases resistant to conservative therapy against coccygodynia the most indicated avenues are therefore
- Local injections: corticosteroids and anaesthetics administered locally, which bring about an improvement in about 60% of cases.
- Manipulation of the coccyx: through specific movements the correct positioning and smoothness of the joint is improved or even restored. In 85% of cases there is an improvement in the clinical picture if the manipulation is carried out in combination with local injections of cortisone and anaesthetic;
- local infiltration with oxygen-ozone (oxygen-ozone therapy), which has an anti-inflammatory effect.
- physiotherapy using tecar therapy and magneto-therapy, stretching exercises and application of heat to improve posture;
- coccygectomy: the surgical removal of the coccyx (in particular its mobile portion), which can affect up to 20% of patients suffering from coccygodynia. The surgical operation determines a clinical improvement in 90% of cases, but it is obviously the most extreme solution, indicated for patients for whom all other therapies have failed with disappearance of the symptom.
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Chronic Pain And Psychotherapy: The ACT Model Is Most Effective
Lumbago: What It Is And How To Treat It
Back Pain: The Importance Of Postural Rehabilitation
Cervical Stenosis: Symptoms, Causes, Diagnosis And Treatment
Pain Therapy For Back Pain: How It Works