Psoriatic arthritis: symptoms, causes and treatment
Psoriatic arthritis (PA) is a chronic inflammatory joint disease (characterized by pain, swelling, heat, joint stiffness, and sometimes redness) associated with the presence of skin psoriasis or familiarity with psoriasis, first described in 1818 by a French physician, Jean Lous Alibert
Psoriatic arthritis is a chronic inflammatory rheumatic disease that:
- affects the joints, causing pain, swelling and stiffness
- affects individuals with skin psoriasis (ongoing or even previous) or with a history of familial psoriasis in first- or second-degree relatives.
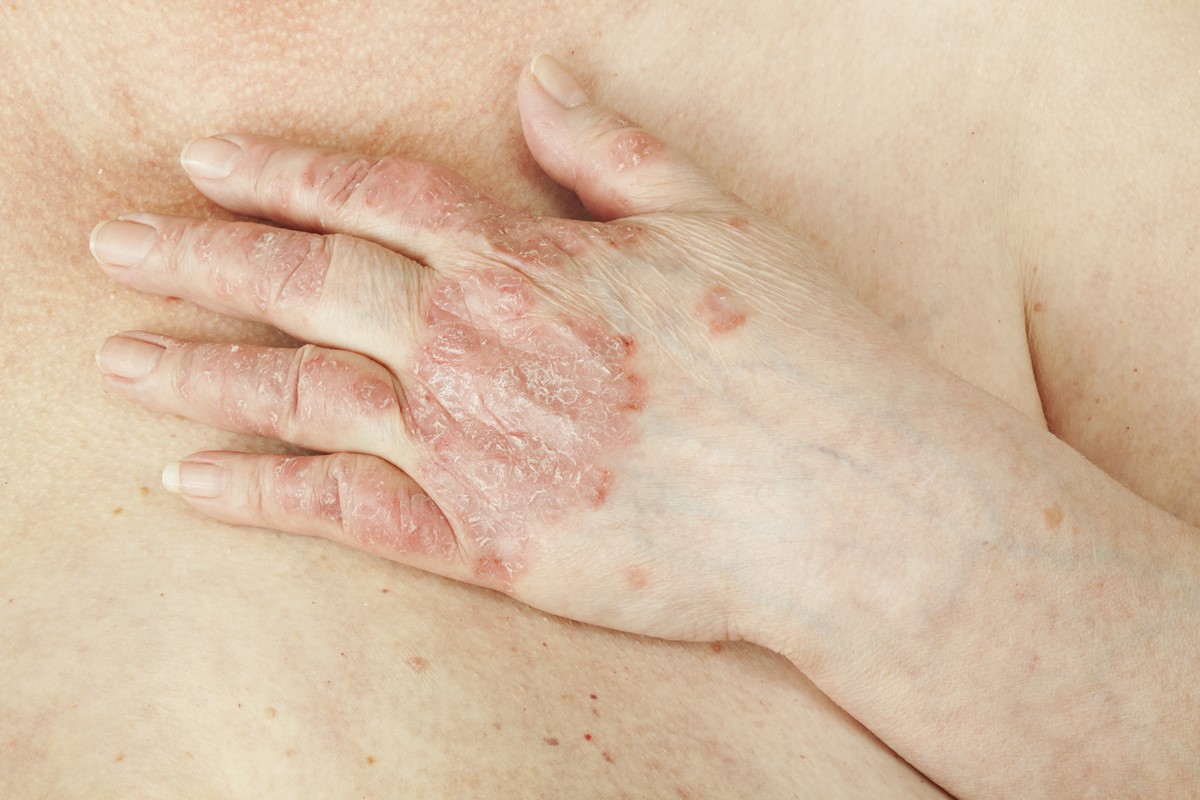
Psoriasis is a skin disease generated by a defect in the immune system and affecting patients with the intermittent appearance of red patches covered with silvery-white scaly plaques in numerous areas of the body, some of which are defined typical sites of psoriatic localization.
Treated rheumatic disease has a prevalence in the general population of 0.3-1% (with no difference between the sexes) and 6-42% in patients with psoriasis (which in turn has a prevalence of 2-3% in the general population).
Family members of patients with psoriatic arthritis are forty times more likely to develop the disease than the rest of the population
The age group with the highest incidence is between 30 and 50 years of age, without significant sex distinction.
In the majority of cases (85%) psoriasis precedes arthritis, in 5-10% of cases the onset is concurrent, and in 5-10% it is arthritis that precedes psoriasis.
The condition is characterized by pain, swelling, heat, and stiffness in the affected joints.
If left untreated, it is a disease that can become disabling because of the significant effects on the quality of life of patients who suffer from it.
Symptoms of psoriatic arthritis
Psoriatic arthritis is characterized by numerous clinical signs and a rather complex course, which is why it is increasingly referred to as “psoriatic disease.”
It may evolve progressively, with mild symptoms, or rapidly, in an acute form.
Manifestations can affect joints on one or both sides of the body.
Psoriatic arthritis usually affects hands and/or feet (especially distally, that is, at the ends of the fingers, near the nail), knees, and ankles.
Involvement of the spine (spondylitis) and sacro-iliac joints (unilateral sacro-ilitis) is possible in 5-10% of cases.
Typically, in cases of psoriatic arthritis, there is at least one of the following symptoms:
- pain, swelling and stiffness (especially in the morning) in one or more joints; sometimes these signs are associated with warmth and redness
- generalized fatigue
- “sausage finger” or dactylitis, which is manifested by homogeneous swelling of a finger of the hand or foot due to inflammation of the tendons and joints of the affected finger
- enthesitis generated by inflammation of the insertion site of tendons and ligaments on bone, such as the Achilles tendon or plantar fascia
- Nail changes (psoriatic onychopathy), such as separation of the nail from the nail bed, streaking and cracking or even loss of the nail itself (onycholysis)
- pain in the sacrum area (lower back, above the coccyx)
- decreased movement
- headaches and pain in the jaw
- talalgia (pain in the heels) and achilles tendinitis
- bursitis (inflammation of the serous bursae)
- ocular involvement, such as conjunctivitis, with redness and itching of the eyes.
The impact of psoriatic arthritis on quality of life depends on the joints affected and the severity of the symptomatology in both psoriasis and the joint condition, phases of active disease may alternate with remission phases.
Persistent inflammation can cause damage to the affected joints and, in the most acute forms, can develop into a disabling condition.
Early diagnosis and treatments are important to avoid or at least slow the effects of the disease.
Causes
Unfortunately, to date, the causes of psoriatic arthritis are not known with certainty, although some possible triggers have been identified.
It appears that the immune system of genetically predisposed individuals may attack joints and other healthy tissues, leading to the onset of an inflammatory process.
Such aggression would be triggered, or otherwise influenced, by particularly stressful events, such as certain environmental elements (prolonged exposure to sunlight), trauma, surgery, and infection.
As mentioned, psoriatic arthritis is generally associated with psoriasis and related familial predisposition.
Recall how psoriasis is a chronic inflammatory skin disease, neither infectious nor contagious, characterized by abnormal and often incomplete keratinization.
At the level of affected skin areas, there are reddened, demarcated, raised patches covered with silver-colored or opalescent scaling (plaques).
The sites most commonly affected by psoriasis are: elbows, knees, palms, soles of the feet, lumbar region, scalp and nails.
In most cases, this skin disease precedes the onset of psoriatic arthritis; however, the opposite situation (onset of the joint condition at the same time as psoriasis or before it) is less common.
While most patients accuse psoriatic arthritis between the ages of 30 and 50, it is also true that the disease can occur at any age and that its onset is unusual in children.
Men and women are equally affected, although female subjects are more likely to develop it, especially following pregnancy or menopause.
Treatment of psoriatic arthritis
Treatment of psoriatic arthritis should be referred to a specialist, to assess likely interactions with other medications as well as possible side effects.
The ultimate goal of the prescribed therapy should be to provide the patient with a good quality of life by controlling symptoms, preventing joint damage, and normalizing function.
The likelihood of success is unquestionably linked to the timing of diagnosis: the earlier the latter, the better.
Pharmacological treatment of symptomatology is based on the use of :
- nonsteroidal anti-inflammatory drugs (NSAIDs) for pain control; their long-term use may result in stomach and intestinal discomfort. Other potential side effects include damage to the kidneys and cardiovascular system
- “disease-modifying anti-rheumatic drugs,” so-called DMARDs, whose action is slower but also longer lasting. Since they are immunosuppressants, they can have side effects on the cells of the blood, liver and kidneys, so periodic tests are needed to check for changes in the function of these organs.
Psoriatic arthritis therapy has undergone profound changes in recent years with the advent of biotechnology drugs, which have targeted action on specific targets responsible for the inflammatory process and not on the entire immune system like DMARDs.
Biotech drugs have proven effective in patients refractory to traditional therapies.
This drug treatment may be indicated in cases where:
- psoriatic arthritis has not responded to at least two different types of DMARDs
- The patient cannot be treated with at least two different types of DMARDs.
Side effects include skin reactions at the injection site, increased susceptibility to infection, nausea, fever, headache, and, more rarely, nervous system disorders, blood disorders, or some cancers.
Finally, physical activity and physiotherapy are also important to maintain joint integrity and function.
Read Also
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Arthrosis: What It Is And How To Treat It
Septic Arthritis: Symptoms, Causes And Treatment
Psoriatic Arthritis: How To Recognize It?
Arthrosis: What It Is And How To Treat It
Juvenile Idiopathic Arthritis: Study Of Oral Therapy With Tofacitinib By Gaslini Of Genoa
Rheumatic Diseases: Arthritis And Arthrosis, What Are The Differences?
Rheumatoid Arthritis: Symptoms, Diagnosis And Treatment
Joint Pain: Rheumatoid Arthritis Or Arthrosis?
The Barthel Index, An Indicator Of Autonomy
What Is Ankle Arthrosis? Causes, Risk Factors, Diagnosis And Treatment
Unicompartmental Prosthesis: The Answer To Gonarthrosis
Knee Arthrosis (Gonarthrosis): The Various Types Of ‘Customised’ Prosthesis
Symptoms, Diagnosis And Treatment Of Shoulder Arthrosis
Arthrosis Of The Hand: How It Occurs And What To Do
Arthritis: Definition, Diagnosis, Treatment, And Prognosis
Rheumatic Diseases: The Role Of Total Body MRI In Diagnosis
Rheumatology Tests: Arthroscopy And Other Joint Tests
Rheumatoid Arthritis: Advances In Diagnosis And Treatment
Diagnostic Tests: Arthro Magnetic Resonance Imaging (Arthro MRI)
Reactive Arthritis: Symptoms, Causes And Treatment


