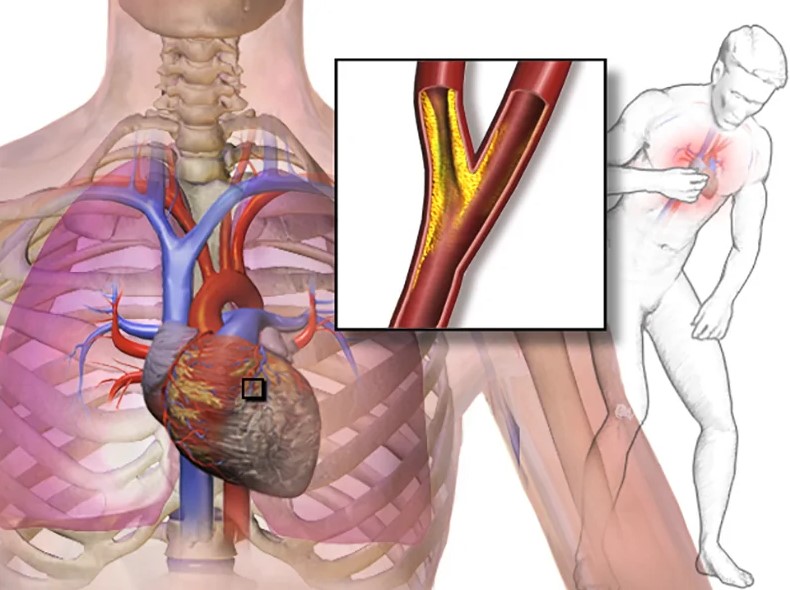
What is ischaemic heart disease and possible treatments
Let’s talk about ischemic heart disease: the heart is the engine of our body and has the task of pumping oxygen-rich blood to the entire body
However, this organ, like all, needs to be adequately ‘supplied’ with blood in order to function.
Sometimes this does not happen due to ischaemic heart disease, a very common disease that includes all conditions in which there is a deficient blood and oxygen supply to the heart.
What is ischaemic heart disease and its causes
Ischaemic heart disease is a very common disease that affects a large part of the world’s population and occurs in all situations in which the heart receives an insufficient supply of blood and oxygen.
The most common cause of ischemic heart disease is precisely the (sudden or gradual) obstruction of the coronary arteries, the arteries that nourish the heart.
In most cases, obstruction of the coronary arteries is caused by atherosclerosis, a typical condition whereby the presence of plaques with a high cholesterol content on the walls of the coronary arteries leads to a narrowing of the vessel’s lumen, resulting in reduced blood flow to the heart.
When the obstruction develops gradually, over months or years, a chronic condition called angina pectoris results.
When the coronary artery obstruction occurs suddenly, myocardial infarction occurs.
Symptoms of ischaemic heart disease
The most frequent and typical symptom of angina pectoris is chest pain, which manifests as oppression and may radiate to the neck, left or right arm.
A characteristic feature of the pain is that it typically appears during exertion or as a result of emotion: in these situations the heart requires a greater supply of energy, a condition that cannot be met if the coronary arteries are obstructed.
Usually in the case of a heart attack, on the other hand, chest pain occurs suddenly and is not related to exertion.
The diagnosis of ischaemic heart disease is made through a series of instrumental examinations such as:
- the electrocardiogram
- the stress test;
- the stress echo;
- myocardial scintigraphy;
- the magnetic resonance stress test.
These are all diagnostic possibilities that allow one to indirectly see the state of health of the coronary arteries.
There are also other modalities through which the coronary arteries can be directly assessed: the first is ANGIO-CT, a non-invasive examination that allows the presence of narrowing of the coronary vessels, secondary to calcifications or atherosclerotic plaques, to be assessed; the second is coronarography, an invasive examination through which the coronary arteries can be directly visualised to view any narrowing and obstructions.
Treatment
If the coronary lesion is moderate, treatment is purely medical, using specific drugs also administered by mouth that have the task of reducing ischaemia of the heart.
If, on the other hand, the lesion is more serious, it may be necessary to proceed with coronary angioplasty or coronary artery bypass surgery, depending on the case.
Coronary angioplasty: a minimally invasive operation
Percutaneous coronary angioplasty involves dilating the coronary artery through the insertion, during coronarography, of a small inflated and expanded balloon at the narrowing of the artery, which is then stabilised with a stent implant (a metal cage with cobalt chrome mesh, coated with a drug capable of preventing so-called ‘re-stenosis’, i.e. the reappearance of plaque in the treated area).
The procedure is performed in the haemodynamic room, following coronarography, under local anaesthesia, with moderate sedation and with the patient awake.
It is a minimally invasive procedure: in most cases, one night’s hospitalisation is sufficient for this treatment.
Although minimally invasive, the procedure in some cases can be complex and require the use of devices to ‘break’ the calcific plaques (using a lithotomy similar to that used for kidney stones) or to ‘mill’ them (with a real miniaturised bur).
Once the operation has been performed and in the first few months following stent implantation, anti-platelet therapy is required to keep the blood particularly fluid to prevent the formation of thrombi and clots.
It is essential that the antiplatelet therapy be continued for as long as the doctor indicates, especially in the first 6 months after surgery.
Coronary bypass surgery, a real surgery
In some cases where the coronary artery disease is extremely extensive and involves all 3 coronary arteries, especially in diabetic patients, it may be necessary to resort to cardiac surgery, i.e. ‘bypass’ surgery.
With this surgery, vascular conduits (of venous or arterial origin) are used to allow direct communication of the upstream portion with the downstream portion of the narrowing (stenosis).
Bypass surgery is a true surgical procedure, requiring general anaesthesia, opening of the chest and in many cases the support of the extra-corporeal circulation (i.e. a machine that works temporarily in place of the heart and lungs, thus allowing surgery on a ‘stopped’ heart).
Lifestyles and ischaemic heart disease
Ischaemic heart disease is certainly linked to a family component: having relatives who have developed this disease leads the patient to a predisposition towards it.
Patients with diabetes mellitus also have a predisposition to the disease, which requires them to undergo regular medical check-ups.
However, it is a multifactorial disease, which is also linked to various bad habits such as:
- cigarette smoking
- sedentary lifestyle;
- hypercholesterolaemia;
- obesity.
These are all risk factors to be kept under control and possibly eliminated, to prevent the possibility of developing or progressing this disease.
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Percutaneous Transluminal Coronary Angioplasty (PTCA): What Is It?
Ischaemic Heart Disease: What Is It?
EMS: Pediatric SVT (Supraventricular Tachycardia) Vs Sinus Tachycardia
Paediatric Toxicological Emergencies: Medical Intervention In Cases Of Paediatric Poisoning
Valvulopathies: Examining Heart Valve Problems
What Is The Difference Between Pacemaker And Subcutaneous Defibrillator?
Heart Disease: What Is Cardiomyopathy?
Inflammations Of The Heart: Myocarditis, Infective Endocarditis And Pericarditis
Heart Murmurs: What It Is And When To Be Concerned
Clinical Review: Acute Respiratory Distress Syndrome
Botallo’s Ductus Arteriosus: Interventional Therapy
Heart Valve Diseases: An Overview
Cardiomyopathies: Types, Diagnosis And Treatment


