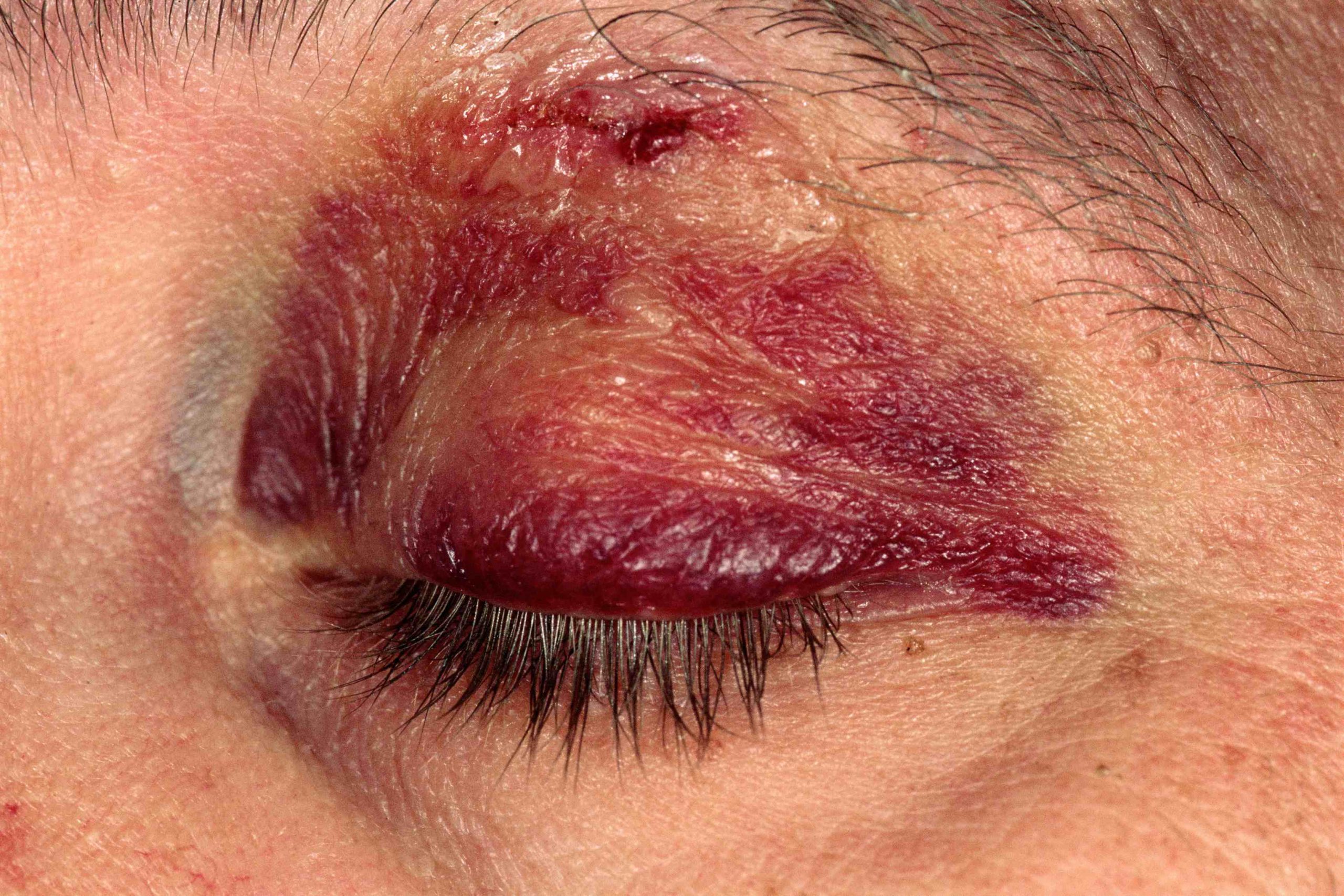
Contusions and lacerations of the eye and eyelids: diagnosis and treatment
Contusions and lacerations of the eyes and eyelids are quite common in emergency rescue operations, so an overview is important
Eyelid lacerations and contusions
Eyelid contusions (resulting in black eyes) have more cosmetic than clinical significance, although sometimes more serious injuries can be associated with them and should not be overlooked.
Uncomplicated contusions are treated with ice packs to prevent oedema during the first 24-48 hours.
Minor lid tears that do not involve the lid margin or tarsal plate can be repaired with 6-0 or 7-0 nylon sutures (or, in children, resorbable material).
Eyelid margin tears should be repaired by an ophthalmic surgeon to ensure correct margins and avoid discontinuity of the lid margin.
Complicated eyelid tears, which include those of the medial portion of the lower or upper eyelid (which may involve the lacrimal canaliculus), full-thickness tears, those in which the patient has palpebral ptosis, and those exposing orbital fat or involving the tarsal plate, should be repaired by an ophthalmic surgeon.
Contusions and lacerations of the eyeball
Trauma can cause the following:
- Conjunctival, anterior chamber and vitreous haemorrhage
- Retinal haemorrhage, retinal oedema or retinal detachment
- Tearing of the iris
- Cataract
- Dislocation of the crystalline lens
- Glaucoma
- Eyeball rupture (tear)
Assessment can be difficult when significant oedema or laceration of the eyelid is present.
Nonetheless, unless the need for immediate eye surgery is obvious (necessitating assessment by an ophthalmologist as soon as possible), the eyelid should be opened, taking care not to put pressure on the eyeball, and as complete an examination as possible should be performed.
As a minimum, the following are assessed:
Visual acuity
- Pupillary morphology and reflexes
- Eye movements
- Anterior chamber depth or haemorrhage
- Presence of red reflex
An analgesic or, after any surgical consent has been obtained, an anxiolytic may be administered to facilitate the objective examination.
Gentle and careful use of an eyelid retractor or eyelid speculum makes it possible to open the eyelids.
If a commercial instrument is not available, the eyelids can be separated with makeshift speculums obtained by opening a paper clip until they are S-shaped, then bending the U-shaped ends up to 180°.
Tearing of the eyeball is suspected with any of the following conditions:
Visible laceration of the cornea or sclera.
- Aqueous humour is escaping (positive Seidel’s sign).
- The anterior chamber is shallow (e.g., making the cornea appear creased) or very deep (due to posterior breakage of the lens).
- The pupil is irregular.
- The red reflex is absent.
If a tear in the eyeball is suspected, the measures that can be taken before an ophthalmologist is available are to apply a protective shield and to counteract a possible infection with systemic antimicrobials, as well as intraocular foreign bodies.
A CT scan should be performed to look for a foreign body and other injuries, such as fractures.
Topical antibiotics are avoided.
Vomiting, which can increase intraocular pressure and contribute to leakage of ocular contents, is suppressed with antiemetic drugs, if necessary.
Because fungal contamination of open wounds is dangerous, corticosteroids are contraindicated until after surgical wound suturing.
Tetanus prophylaxis is indicated for open eyeball wounds.
Very rarely, after a laceration of the eyeball, the contralateral non-traumatised eye becomes inflamed (sympathetic ophthalmia) and may lose vision up to blindness if left untreated.
The mechanism is an autoimmune reaction; corticosteroid drops can prevent the process and can be prescribed by an ophthalmologist.
Hyphema (anterior chamber haemorrhage)
Hyphema can be followed by recurrent haemorrhages, glaucoma and haemorrhagic infarction of the cornea, all of which can cause permanent loss of vision.
Symptoms are those of the associated lesions unless the hyphema is large enough to prevent vision.
Direct inspection typically reveals blood stratification or the presence of a clot or both within the anterior chamber.
Stratification looks like a meniscus-shaped blood layer in the declivity (usually the lower part) of the anterior chamber.
Microhyphema, a less severe form, can be seen on direct inspection as an anterior chamber opacity or on slit-lamp examination as suspended red blood cells.
An ophthalmologist should attend to the patient as soon as possible.
The patient is placed in bed with the head raised 30-45° and an eyecup is placed to protect the eye from further trauma.
Patients at high risk of haemorrhagic recurrence (e.g., patients with extensive hyphemas, haemorrhagic diathesis, anticoagulant use, or drepanocytosis), with poor control of intraocular pressure, or with poor compliance with recommended treatment, should be admitted.
Oral and topical NSAIDs are contraindicated because they may contribute to recurrent bleeding.
Intraocular pressure may increase acutely (within hours, usually in patients with drepanocytosis or sickle cell trait), or months and years later.
Therefore, intraocular pressure should be monitored daily for several days and then regularly in the following weeks and months, and if symptoms develop (e.g. eye pain, reduced vision, nausea, similar to the symptoms of acute angle-closure glaucoma).
If pressure increases, timolol 0.5% twice/day, brimonidine 0.2% or 0.15% twice/day, or both are administered.
Response to treatment is dictated by pressure, which is often monitored every 1-2 h until it is controlled or a significant reduction is demonstrated; thereafter, it is usually monitored 1 or 2 times/day.
Midriatic drops (e.g. scopolamine 0.25% 3 times/day or atropine 1% 3 times/day for 5 days) and topical corticosteroids (e.g. prednisolone acetate 1% 4 to 8 times/day for 2 to 3 weeks) are often administered to reduce inflammation and scarring.
If bleeding recurs, an ophthalmologist should be consulted for management.
Administration of aminocaproic acid 50 to 100 mg/kg orally every 4 h (not exceeding 30 g/day) for 5 days or tranexamic acid 25 mg/kg orally given 3 times/day for 5 to 7 days may reduce recurrent bleeding, and myotonic or mydriatic drugs should also be prescribed.
Rarely, recurrent bleeding with secondary glaucoma requires surgical evacuation of the blood.
Injuries and lacerations, but also orbital fracture
Orbital fracture occurs when blunt trauma pushes the orbital contents through one of the more fragile walls of the orbit, typically the floor.
Fractures of the medial wall and roof can also occur.
Orbital haemorrhage can cause complications such as infraorbital nerve entrapment, eyelid oedema and ecchymosis.
Patients may have orbital or facial pain, diplopia, enophthalmos, hypoesthesia of the cheek and upper lip (due to infraorbital nerve injury), epistaxis, and subcutaneous emphysema.
Other facial injuries or fractures should also be excluded.
Diagnosis is best made with the use of thin-layer CT through the facial skeleton.
If ocular motility is impaired (e.g., causing diplopia), the extraocular muscles should be assessed for signs of entrapment.
If there is diplopia or cosmetically unacceptable enophthalmos, surgical repair may be indicated.
Patients should be told to avoid blowing their noses to prevent orbital compartment syndrome from air reflux.
The use of a topical vasoconstrictor for 2 to 3 days may relieve epistaxis.
Oral antibiotics may be used if patients have sinusitis.
Orbital compartment syndrome
Orbital compartment syndrome is an ophthalmic emergency.
Orbital compartment syndrome occurs when intraocular pressure suddenly increases, usually due to trauma, causing haemorrhage.
Symptoms may include sudden loss of vision, as well as diplopia, eye pain, eyelid swelling, and bruising.
Objective examination may show decreased vision, chemosis, afferent pupillary defect, proptosis, ophthalmoplegia, and elevated intraocular pressure.
The diagnosis is clinical and treatment should not be delayed for imaging.
Treatment consists of immediate lateral cantholysis (surgical exposure of the lateral canthal tendon with incision of its inferior branch) followed by:
- Monitoring with possible hospitalisation with elevation of the bed head to 45°.
- treatment of elevated intraocular pressure as in acute angle-closure glaucoma
- Reversal of any coagulopathy
- Prevention of further increase in intraocular pressure (prevention or reduction of pain, nausea, cough, tension, severe hypertension)
- Application of ice or cold packs
Read Also:
Emergency Live Even More…Live: Download The New Free App Of Your Newspaper For IOS And Android
Autoimmune Diseases: The Sand In The Eyes Of Sjögren’s Syndrome
Corneal Abrasions And Foreign Bodies In The Eye: What To Do? Diagnosis And Treatment
Wound Care Guideline (Part 2) – Dressing Abrasions And Lacerations


