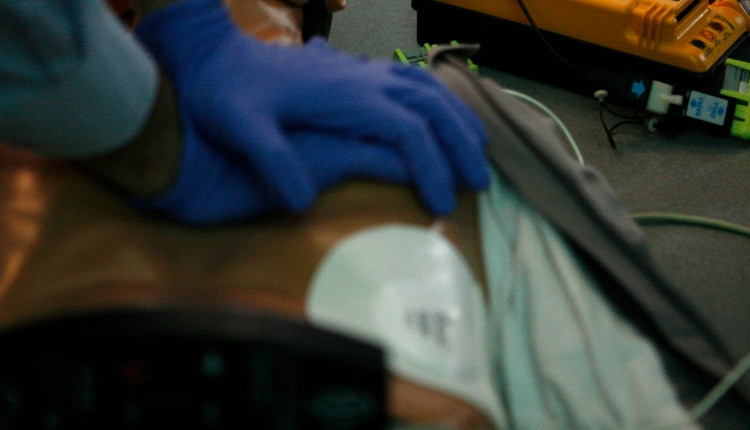
CPR - Are we compressing in the right position? Probably not!
CPR is the best known life-saving practice. The cardiopulmonary resuscitation helps compressing the heart and, in particular, the Left Ventricle in order to generate a stroke volume and perfuse the outflow tract to the brain and the rest of the organs.
This is what CPR is used to. As many do, the CPR is performed by compressing the center of the chest. But are you sure that it is enough? Do you think are you performing it right?
Well, we are pleased to introduce the following article edited by Dr. Rugna Mario about how to perform a perfect CPR.
The objective of chest compressions in CPR is to compress the heart and in particular the Left Ventricle (LV) to generate a stroke volume (SV) trough the Left Ventricular Outflow Tract (LVOT) to perfuse the heart the brain and the rest of the organs.
Performing CPR we blindly compress the center of the chest on the sternum approximately at the level of intermammillar line (as recommended by the 2015 CPR Guidelines) but we risk to apply the Area of Maximum Compression (AMC) not only on the LV but also on the Aortic Valve (AV) and the Ascending Aorta (AA) closing them and generating less (or none) LV stroke volume but just an ineffective retrograde flow.
Depending on how much the AMC is positioned on the left ventricle or on the aortic part of the heart chest compressions are respectively more or less efficacious to perfuse the brain the heart and the organs.
This is not just theory but was demonstrated in animal and human studies (See References links at the bottom).
In particular Sung Oh Hwang and coll. in the article “Compression of the Left Ventricular Outflow Tract During Cardiopulmonary Resuscitation” observe that”the magnitude of compression of the left ventricle is more significant when a maximal compression occurs at the LVOT than when a maximal compression occurs at the ascending aorta during external chest compression“. They also determined “that external chest compression at the hand position currently recommended by the AHA guidelines compresses the LVOT or the ascending aorta.” and conclude that “(….) the compression location currently recommended by the AHA guidelines may not be effective in generating forward blood flow during CPR.”(….) it is possible that compressing the caudal part of the sternum will improve the quality of CPR and reduce rescuer fatigue.“
The investigators stated also that the Optimal Compression Point (OCP) cannot be definitively addressed because it depends on many variables and varies from patient to patient depending “on the configuration of the heart in the thorax.”
All those findings were assessed using Trans Esophageal Echocardiography (TEE) inserted during CPR in real cases scenarios to visualise the heart to measure the LV stroke volume in order to find the best OCP.


